From the Editor
This week, we focus on alcohol, with two papers and a news article. Obviously, alcohol isn’t new – distilling probably started in the 13th century – but the three selections offer fresh and important information that is clinically relevant.
In the first selection, we consider the link to cancer. In a new Lancet Oncology paper, Harriet Rumgay (of the International Agency for Research on Cancer) and her co-authors conduct a population-based study. “Globally, about 741 000, or 4.1%, of all new cases of cancer in 2020 were attributable to alcohol consumption.” We review the big paper and mull its clinical implications.
In the second selection, Dr. Daniel Myran (of the University of Ottawa) and his co-authors look at ED visits due to alcohol. Drawing on administrative data, they write: “We found that that current patterns and temporal trends in ED visits due to alcohol show large disparities between urban and rural regions of Canada and by socioeconomic status.”
And in the third selection, reporter Anahad O’Connor writes about alcohol use disorder for The New York Times. In this highly readable article, he focuses on the struggles of a retired manager: “But this past winter, with the stress of the pandemic increasingly weighing on him, he found himself craving beer every morning, drinking in his car and polishing off two liters of Scotch a week.” O’Connor writes about several resources that may be helpful to patients and their families.
DG
Selection 1: “Global burden of cancer in 2020 attributable to alcohol consumption: a population-based study”
Harriet Rumgay, Kevin Shield, Hadrien Charvat, et al.
The Lancet Oncology, 13 July 2021 Online First
Alcohol use is associated with a vast range of injuries and diseases, including cancer, and is a leading risk factor for the global burden of disease. The consumption of alcoholic beverages is causally linked to cancers of the upper aerodigestive tract (oral cavity, pharynx, larynx, and oesophagus) and cancers of the colon, rectum, liver, and female breast. Together, these cancers contributed 6.3 million cases and 3.3 million deaths globally in 2020 (data from the GLOBOCAN 2020 database).
Previous estimates of the contribution of alcohol to the burden of cancer have been published, but patterns of alcohol consumption continue to change over time across world regions. Alcohol consumption per capita has decreased in many European countries, especially those in eastern Europe, whereas alcohol use is on the rise in Asian countries, such as China, India, and Vietnam, and in many countries in sub-Saharan Africa. With these changes in alcohol consumption and more recent cancer incidence data, new estimates of the alcohol-attributable burden of cancer are warranted.
So begins a paper by Rumgay et al.
Here’s what they did:
- The authors conducted a population-based study.
- They considered population attributable fractions (PAFs) – using “a theoretical minimum-risk exposure of lifetime abstention and 2010 alcohol consumption estimates from the Global Information System on Alcohol and Health combined with corresponding relative risk estimates” – “applied to cancer incidence data from GLOBOCAN 2020 to estimate new cancer cases attributable to alcohol.”
- They calculated “the contribution of moderate (<20 g per day), risky (20–60 g per day), and heavy (>60 g per day) drinking to the total alcohol-attributable cancer burden, as well as the contribution by 10 g per day increment (up to a maximum of 150 g). 95% uncertainty intervals (UIs) were estimated using a Monte Carlo-like approach.”
Here’s what they found:
- Total cancers: an estimated 741 300 or 4.01% of all new cases of cancer in 2020 were attributable to alcohol consumption.
- Gender: males accounted for 568 700 or 76.7% of these cancer cases.
- Types of cancer: cancers of the esophagus (189 700 cases), liver (154 700 cases), and breast (98 300 cases) were the most common.
- Cancer and drinking patterns: heavy drinking (346 400, or 46.7%) and risky drinking (291 800, or 39.4%) were the most tied to cancer; that said, moderate drinking (103 100, or 13.9%) was problematic.
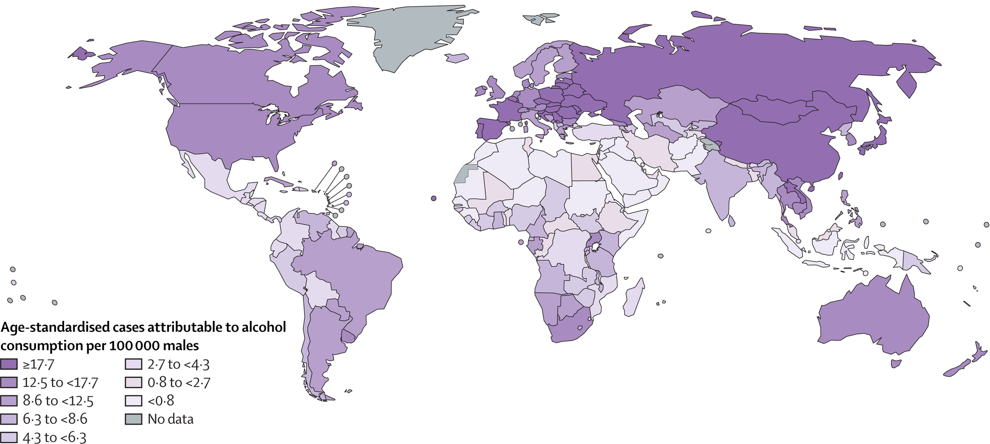
- Geography: “PAFs were lowest in northern Africa and western Asia in both sexes, and highest among males in eastern Asia and central and eastern Europe, and among females in central and eastern Europe, Australia and New Zealand, and western Europe.”
A few thoughts:
- This is a good study.
- Obviously, this summary provides a rough overview of a thoughtful analysis.
- How do the findings compare to past work? “Our estimated global PAF was lower than the previous global estimates of 5.5% of cancer cases in 2012…” So is this good news? The authors suggest it may be: “This difference could be due to genuine decreases in consumption of alcohol in several world regions, such as in southern Europe and central and eastern Europe…”
- Like all papers, there are limitations. The authors note that the analysis didn’t take into account of the synergistic effects of tobacco and alcohol.
- What’s the Canadian context? I highlight local stats from another publication: “In Canada, alcohol use was linked to 7,000 new cases of cancer in 2020, including 24% of breast cancer cases, 20% of colon cancers, 15% of rectal cancers, and 13% of oral and liver cancers.”
- How to understand the risk of cancer with alcohol use (particularly heavy use)? The CDC suggests that 40% of cancers in the United States are linked to cigarettes. Though this is something of an apples-to-oranges comparison, the point is that alcohol isn’t as carcinogenic as tobacco – but is carcinogenic all the same.
- What’s the clinical relevance? We often speak to people about the risks of alcohol. How often do we mention cancer? And, in people with alcohol use disorder, should we be extra vigilant for the possibility of cancer?
The full Lancet Oncology paper can be found here:
https://www.thelancet.com/journals/lanonc/article/PIIS1470-2045(21)00279-5/fulltext
Selection 2: “Socioeconomic and Geographic Disparities in Emergency Department Visits due to Alcohol in Ontario: A Retrospective Population-level Study from 2003 to 2017”
Daniel Myran, Amy Hsu, Elizabeth Kunkel, et al.
The Canadian Journal of Psychiatry, 13 July 2021 Online First
In Canada, there is a general understanding that certain sociodemographic groups experience a higher burden of alcohol harms (e.g., low-income individuals and middle-aged men) and larger increases in harms over time (e.g., women and young adults). However, there is a limited knowledge about alcohol-related harms in rural populations in Canada as well as less understanding of trends in socioeconomic and geographic disparities over time. In light of a growing epidemic of alcohol-related harms, such data are urgently needed to identify gaps in the delivery of clinical services and better target alcohol control policies based on evidence.
So notes Myran et al. in a new paper.
Here’s what they did:
- They conducted a retrospective population-level cohort study in Ontario.
- They considered ED visits due to alcohol between 2003 and 2017, linking to administrative data, including the National Ambulatory Care Reporting System database.
- They then calculated “annual age- and sex-standardized, and age- and sex-specific rates of ED visits and compared overall patterns and changes over time between urban and rural settings and income quintiles.”
Here’s what they found:
- There were 829 662 ED visits due to alcohol over 15 years.
- ED visits: “Rates of ED visits due to alcohol were greater for individual living in the lowest- compared to the highest-income quintile neighbourhoods…”
- Rural vs. urban: “Rates of ED visits due to alcohol were significantly greater in rural settings (56.0 per 10 000 individuals…) compared to urban settings (44.8 per 10 000 individuals…), particularly for young adults.
A few thoughts:
- This is a good study.
- The core findings are hardly surprising.
- The authors did consider changes over time. “Annual rates increased significantly in all 24 subgroups over our study period. The increases in visits, between 2003 and 2017, were greater in rural compared to urban settings (82% vs. 68% increase in age- and sex-standardized rates); this may be attributable to the relatively larger increase in age-standardized rates among women (114% rural vs. 85% urban) compared to men (60% rural vs. 63% urban).”
- The authors note: “Overall, the burden of alcohol on the health system in Canada appears to be increasing particularly in rural regions.” The implications for public policy are clear.
The full CJP paper can be found here:
https://journals.sagepub.com/doi/10.1177/07067437211027321
Selection 3: “Alcohol Abuse Is on the Rise, but Doctors Too Often Fail to Treat It”
Anahad O’Connor
The New York Times, 12 July 2021
Like many people who struggle to control their drinking, Andy Mathisen tried a lot of ways to cut back.
He went through an alcohol detox program, attended Alcoholics Anonymous meetings, and tried using willpower to stop himself from binge drinking. But this past winter, with the stress of the pandemic increasingly weighing on him, he found himself craving beer every morning, drinking in his car and polishing off two liters of Scotch a week.
Frustrated, and feeling that his health and future were in a downward spiral, Mr. Mathisen turned to the internet and discovered Ria Health, a telehealth program that uses online coaching and medication to help people rein in their drinking without necessarily giving up alcohol entirely.
After signing up for the service in March, he received coaching and was given a prescription for naltrexone, a medication that diminishes cravings and blunts the buzz from alcohol.
So begins an article by O’Connor.
He reviews the literature:
- “Last month, a nationwide study by researchers at the Washington University School of Medicine in St. Louis found that about 80 percent of people who met the criteria for alcohol use disorder had visited a doctor, hospital or medical clinic for a variety of reasons in the previous year. Roughly 70 percent of those people were asked about their alcohol intake. Yet just one in 10 were encouraged to cut back on their drinking by a health professional, and only 6 percent received any form of treatment.”
- “Research suggests that among all the people with alcohol use disorder who try to quit drinking every year, just 25 percent are able to successfully reduce their alcohol intake long-term.”
- “In a study published last month, scientists at the N.I.H. found that just 1.6 percent of the millions of Americans with alcohol use disorder had been prescribed a medication to help them control their drinking.”
The article describes the treatment of Mathisen: “After signing up for the service in March, he received coaching and was given a prescription for naltrexone, a medication that diminishes cravings and blunts the buzz from alcohol. The program accepts some insurance and charges $350 a month for a one-year commitment for people who pay out of pocket. Since he started using it, Mr. Mathisen has reduced his drinking substantially, limiting himself to just one or two drinks a couple days a week.”
The article closes by mentioned resources available to patients.
- “The National Institute on Alcohol Abuse and Alcoholism has a free website called Rethinking Drinking that can help you find doctors, therapists, support groups and other ways to get treatment for a drinking problem.”
- “Cutback Coach is a popular app that helps people track their alcohol intake and set goals and reminders so they can develop healthier drinking habits. The service allows people to track their progress and sends out daily reminders for motivation. The cost is $79 if you pay annually, $23 per quarter or $9 a month.”
- “Moderation Management is an online forum for people who want to reduce their drinking but not necessarily abstain. The group offers meetings, both online and in person, where members can share stories, advice and coping strategies. It also maintains an international directory of ‘moderation-friendly’ therapists.”
A few thoughts:
- This is a good article.
- I note the cultural shift: not that long ago, substance problems were portrayed as moral failings, not medical diseases.
- It’s interesting to note how many options people have in terms of treatment – yes, medications help, but also apps and online support.
The full NYT article can be found here:
https://www.nytimes.com/2021/07/12/well/live/alcohol-abuse-drinking-treatment.html
Reading of the Week. Every week I pick articles and papers from the world of Psychiatry.


Recent Comments