From the Editor
I don’t quite remember when I changed my interview questions, but at some point – more than a decade ago – I stopped assuming that if I asked about street drugs, patients would tell me about cannabis. Long before legalization, people stopped seeing cannabis as illicit. Today, not only is cannabis legal for recreational use, many see it as a drug to be taken for their health.
In a new Canadian Journal of Psychiatry paper, the authors write about cannabis use for medicinal purposes among Canadian university students. Drawing on a survey, they find wide use – but not exactly the use that follows the guidelines.
We also consider two other pieces: an obituary for Dr. Richard Green, a prominent psychiatrist who challenged the DSM’s inclusion of homosexuality, and an interview with Dr. Scott Gottlieb, the outgoing FDA Commissioner, who worries about e-cigarettes.
 Use – but medicinal use?
Use – but medicinal use?
Enjoy these selections.
And an invitation: the Reading of the Week series invites guest contributions. If this is of interest to you, please let me know.
DG
Selection 1: “Cannabis Use for Medicinal Purposes among Canadian University Students”
Jacqueline M. Smith, Joel Mader, Andrew C. H. Szeto, Amelia M. Arria, Ken C. Winters, T. Chris R. Wilkes
The Canadian Journal of Psychiatry, 2 January 2019 Online First

The number of registered medicinal cannabis users in Canada has more than tripled since 2016. The medicinal cannabis market has become increasingly competitive, with medicinal dispensaries promoting cannabis for an array of medical ailments ranging from mental illnesses to physical conditions. Although dispensaries promote cannabis as a panacea for numerous disorders, the scientific evidence supporting its efficacy is often overstated or insufficient, and use has been associated with adverse outcomes. Recently, the Canadian clinical practice guidelines and National Academies of Science, Engineering, and Medicine in the United States recommended limiting medicinal cannabis to a narrow subset of medical conditions, including palliative and neuropathic pain, chemotherapy-induced nausea and vomiting, and spasticity due to multiple sclerosis.
Although general authorization guidelines have been proposed, little is known about how medicinal cannabis use may differ among subpopulations, including emerging adults (18-25 years of age).
So begins a paper by the University of Calgary’s Jacqueline M. Smith and her co-authors.
Here’s what they did:
- They surveyed 4 000 university students.
- The questionnaire was a cross-sectional web-survey that took 15-25 minutes to complete.
- Questions focused on recreational and medicinal use of cannabis.
Here’s what they found:
- 2 215 people responded to the survey, a response rate of 55.3%.
- “Regarding motives, 56% used only recreationally, 18.1% used both medicinally and recreationally, 3% were medicinal only, and 23.2% did not endorse the criteria for either motive. In total, 21.1% of lifetime users reported medicinal cannabis use and 74.1% reported recreational use.”
- “The majority of medicinal users used infrequently and more than a third (35%) reported that medicinal cannabis use was authorized by a health care professional.”
- In terms of use, see figure below.
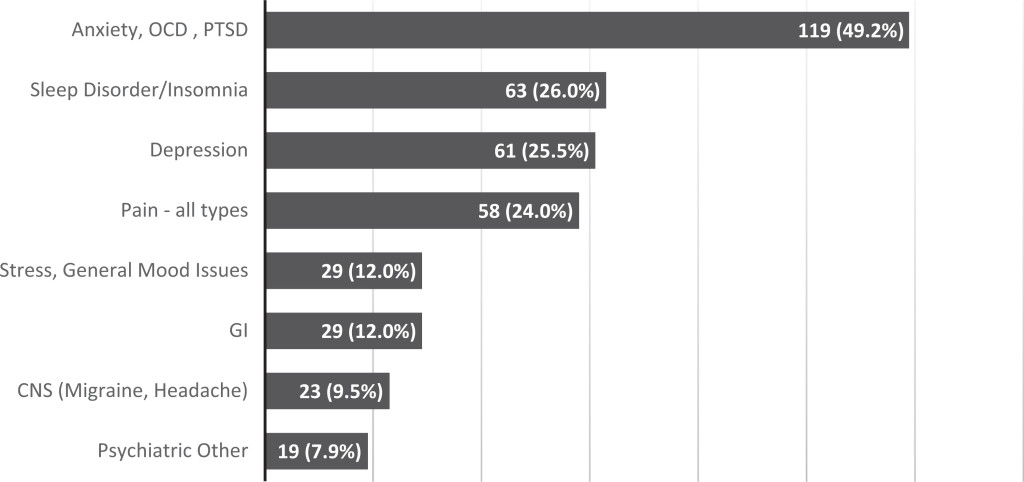
The authors write:
Lifetime cannabis use for medicinal purposes is relatively common in this university sample (∼11%). Many students reported medicinal cannabis use to relieve anxiety or depression, and one-third replaced a traditional treatment with cannabis.
In a recent conversation, a legal scholar questioned if the government’s decision to allow cannabis for medicinal use then for recreational use was problematic, and that we would have been better off simply legalizing the latter. It’s a reasonable thought – though life isn’t spent looking in the rearview mirror. How to move forward? This survey suggests that many young Canadians see cannabis as medicinal – and us clinicians need to address that in our practices.
The full paper can be found here: https://journals.sagepub.com/doi/full/10.1177/0706743718818420
Selection 2: “Dr. Richard Green, 82, Dies; Challenged Psychiatry’s View of Homosexuality”
Benedict Carey
The New York Times, 17 April 2019
![]()
Dr. Richard Green, one of the earliest and most vocal critics of psychiatry’s classification of homosexuality as a mental disorder, died on April 6 at his home in London. He was 82. The cause was esophageal cancer, his son, Adam Hines-Green, said.
Dr. Green, who was also a forceful advocate for gay and transgender rights in a series of landmark discrimination trials, became aware of the marginalization of people because of their sexual and gender identities while training to be a doctor at Johns Hopkins University in Baltimore, a leader in the study of sexuality.
In 1972, shortly after completing his specialty in psychiatry, he defied the advice of colleagues and wrote a paper in The International Journal of Psychiatry questioning ‘the premise that homosexuality is a disease or a homosexual is inferior.’
So begins an obituary by reporter Benedict Carey.
Carey describes the life and career of Dr. Green, a New Yorker who became a lawyer, who then moved to London, where he studied medicine.
It notes his long advocacy and academic interests.
- Green argued against the inclusion of homosexuality in the Diagnostic and Statistical Manual.
- “Dr. Green continued his advocacy throughout his career, appearing as an expert witness on behalf of gay or transgender people in more than a dozen trials.”
- “In 1975, he founded the International Academy of Sex Research and became the first editor of its journal, Archives of Sexual Behavior, a position he held until 2002.”
The article discusses his campaign against the premise that homosexuality is a disease. Columbia University’s Jack Drescher notes: “Those were times when, if you spoke up in support of homosexuals, people immediately thought that you were secretly homosexual yourself, or had unresolved sexual issues, Richard was very much heterosexual, and it took a lot of courage to argue for gay people.”
Carey makes a passing mention of other advocates, including Dr. Robert Spitzer. (A more comprehensive consideration of this topic can be found in Dr. Jeffery Lieberman’s book on the history of psychiatry, Shrinks.) In reading this obituary, we are reminded that these debates occurred not so long ago.
The NYT piece is here: https://www.nytimes.com/2019/04/17/obituaries/dr-richard-green-dead.html?searchResultPosition=6
Selection 3: “Scott Gottlieb’s last word as FDA chief: Juul drove a youth addiction crisis”
Julia Belluz
Vox, 5 April 2019
It’s not that often that you hear a top Trump official unabashedly blaming a US company for a health crisis. But that’s exactly what FDA chief Scott Gottlieb did Tuesday in an interview during his final week in office.
‘The dramatic spike of youth [vaping] — that was driven in part at the very least if not largely by Juul,’ the maker of hugely popular vape products, Gottlieb told Vox by phone. ‘I hope they recognize the problem that’s been created has been created largely by their product.’
Gottlieb joined the Trump administration in 2017, hoping to use policy to further reduce cigarette smoking, still the leading cause of preventable death in the US.
But then the teen vaping epidemic – what he calls an ‘addiction crisis’ – exploded under his watch. By 2018, the number of high school seniors who say they vaped nicotine in the past 30 days doubled over the previous year – from 11 percent to nearly 21 percent, according to the National Institutes of Health survey. That was the largest increase ever recorded in any substance of the survey’s 43-year history.
Writing for Vox, Belluz interviews Dr. Gottlieb.
He makes several points about vaping and regulations:
- By 2018, Juul Labs took over three-quarters of the US e-cigarette market.
- “There’s no question the Juul product drove a lot of the youth use… I’m not willing to concede the point that the Juul product was responsible – at least in part – for the sharp uptick in youth use.”
- “If you go back and look at their marketing campaigns from 2015 and 16, it’s hard not to look at that marketing and conclude that’s it’s not going to be appealing to a youth, to a teenager. It certainly in my view had some impact on creating the problem we have now.”
Though he acknowledges the possibility that smokers may have an easier time quitting with e-cigarettes, Dr. Gottlieb remains concerned about use in teens, and calls for more careful monitoring and possible regulations.
Dr. Gottlieb makes good points – though the issue is complicated. As was discussed in a past Reading, there is evidence that e-cigarettes are useful for smoking cessation – thus there is a public health opportunity (cessation) but also a significant problem (youth addiction).
The interview can be found here: https://www.vox.com/science-and-health/2019/4/5/18287073/vaping-juul-fda-scott-gottlieb
A recent Reading on smoking cessation and e-cigarettes can be found here: http://davidgratzer.com/reading-of-the-week/reading-of-the-week-do-e-cigarettes-help-with-smoking-cessation-the-new-nejm-paper/.
Reading of the Week. Every week I pick articles and papers from the world of Psychiatry.
Recent Comments