From the Editor
How will the pandemic impact mental health? Will we see more people with depression and PTSD? What about suicides?
In a recent JAMA Psychiatry paper, Mark A. Reger (of the University of Washington) and his co-authors argued that we may see a “perfect storm” with COVID-19, increasing the risk of suicide. A BMJ blog speculated that we could have a “pandemic after the pandemic,” as mental health problems grow even as the virus fades.
This week, we have two selections; the first focuses on suicide and the pandemic. Using an innovative approach – that is, considering Google searches for suicide and related terms, as a proxy for completions – the authors draw on American and international data. In a new Canadian Journal of Psychiatry paper, Dr. Mark Sinyor (of the University of Toronto) and his co-authors find surprisingly “that the initial stages of the pandemic were accompanied by a substantial reduction in searches related to suicide, anxiety, and hopelessness with no change in searches for depression.”

In the second selection, Dr. Justin L. Bullock (of the University of California, San Francisco) discusses suicide in The New England Journal of Medicine. The young doctor is very personal, describing his own struggles with mental illness. “‘I’m starting to get depressed,’ I told my sister emotionlessly. She began to cry, probably flashing back to the last time I was severely depressed, attempted suicide, and ended up in the ICU. I told her I was sad that my 2-year-old niece wouldn’t remember me. ‘Do you think I would ever let her forget you?’ she responded. We both cried.”
DG
Selection 1: “Changes in Suicide and Resilience-related Google Searches during the Early Stages of the COVID-19 Pandemic”
Mark Sinyor, Matthew J. Spittal, Thomas Niederkrotenthaler
The Canadian Journal of Psychiatry, 11 June 2020 Online First
![]()
Pandemics such as the 2019 coronavirus (COVID-19) outbreak have the potential to negatively impact mental health, which may, in turn, influence suicide rates. Due to the substantial lag before mortality data become available, it will be some time before that can be investigated. More readily available proxy indicators, such as Google search trends, may be of value both for early characterization of the impact of COVID-19 on suicide and in formulating an early public health response. However, this has never been tested in the context of a pandemic. We aimed to characterize changes in suicide-related searches worldwide and in the United States (the country with the most reported COVID-19 cases to date) to identify potential early indications of impact on suicide which can later be compared to mortality data.
Here’s what they did:
- They used internet search data (with Google Trends) for the word “suicide” and several related terms.
- The pre-COVID period was the five years up to 28 February 2020; the COVID-19 period was 1 March to 4 April 2020.
- They then did a time series analyses for each term; statistical analyses were done (generalized linear model using the Poisson family).
Here’s what they found:
- There were significant reductions in searches for the word “suicide” both worldwide (-12%) and in the United States (-17%).
- The same was observed for “suicide methods”: worldwide: -39%; United States: -36%.
- Changes in searches for “how to commit suicide” and “how to kill yourself” were not significant.
- The figure below shows the queries worldwide.

Taken together, these findings assist in developing a conceptual model for the world’s initial reaction to the crisis. They suggest that, as may have been expected, the pandemic has triggered an increased focus on finding ways to survive and to overcome challenges but possibly also more negative emotionality. The latter may be perceived by many as a natural reaction to stressful circumstances rather than a pathological one (i.e., “sadness” rather than “depression”). Both a focus on survival and/or a perception that suffering is expected/appropriate given the circumstances could plausibly lead to a reduction in societal and individual focus on suicide. This, in turn, could suggest a reduction in suicide-related outcomes such as suicide attempts and deaths although that remains to be studied.
A few thoughts:
- This is an interesting study.
- The authors have a clever way of measuring (indirectly) suicide by looking at Google searches.
- Clever – but meaningful? The authors draw on the work of John W. Ayers (of San Diego State University), who has termed the approach “quasiexperimental” in one of his papers. But Ayers is able to show that internet searches are connected to completed suicides, citing past work that analyzed suicide data from Taipei City, Taiwan, and corresponding local internet search trend data.
- Is there any data that supports this finding? There is: from Japan. Relatively recent Japanese data shows a decline in suicide completions at the start of the pandemic.
A Guardian article on the topic can be found here: https://www.theguardian.com/world/2020/may/14/japan-suicides-fall-sharply-as-covid-19-lockdown-causes-shift-in-stress-factors
- Should we be surprised by the Japanese data? Maybe. Suicide rates tend to go up during difficult economic times, but decline during times of war (one explanation: such conflicts stoke feelings of national unity and purpose). Has the pandemic followed the latter pattern?
- In a new paper, Dr. Roger S. McIntyre and Yena Lee (both of the University of Toronto) make the argument that suicides will increase, drawing on historical data. Theyconsider past economic recession, and suggest scenarios depending on unemployment – that is, if we consider the rise of suicides during past periods of higher unemployment, can we then project completions in 2020 and 2021?
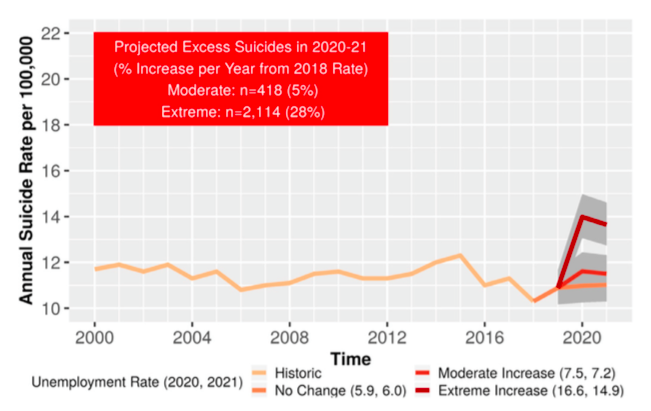
They draw on real data. But suicide is multifactorial, and they only consider unemployment. As the authors acknowledge: “We recognize that no single variable accounts for completed suicide within individuals or populations.”
The full paper can be found here: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7236718/#!po=35.1852
- Could both sets of authors be right in their conclusions? Could suicide trend down in the early days of this pandemic (national unity and purpose), only to trend up later (economic woes)?
- The use of Google data is creative – a dataset that didn’t exist just a few short years ago. There is something exciting about the approach, giving us possible insights into a problem months before coroners’ reports are available. We can wonder if Google search data could eventually lead to real-time interventions. And, of course, we should mull the implications for privacy.
The Canadian Journal of Psychiatry research letter is here: https://journals.sagepub.com/doi/full/10.1177/0706743720933426
Selection 2: “Suicide – Rewriting My Story”
Justin L. Bullock
The New England Journal of Medicine, 26 March 2020

Intern year is a marathon. It’s an analogy I’ve heard often, and one that resonates with the runner in me. Both intern year and marathons have a way of revealing vulnerabilities and breaking even the strongest among us. Overwhelmed by sick patients, night shifts, goals-of-care meetings, medical hierarchy, microaggressions, and feelings of inadequacy, even the most solid interns can falter. As an intern with a mental illness, I approached the starting line knowing that at some point my vulnerabilities would be exposed and that hitting the wall was inevitable. I didn’t know when, but if my history of mental illness was any indicator, my crash would be bad.
So begins a paper by Dr. Bullock.
He notes his strong start to residency:
“My year started off perfectly. I matched at my first-choice program, loved my intern class, and had a paper published, and my mentor and I were asked to give departmental grand rounds. Yet the bipolar mind is fickle, and happiness and accomplishment can quickly fade into pain and suffering.”
But he has bipolar, and sinks into a depressive episode:
“As I get sicker, depression’s seductive voice begins to sound rational. Justin, you aren’t strong enough to take another depression, just kill yourself now before it gets worse. I titrated my medications, hoping to correct my brain chemistry.”
He writes about the deep challenges he faces – and the challenges of the system, even for someone as connected as he is. He opts to go to hospital.
“My program’s response to my hospital admission was far from perfect. After I had disclosed my struggle, it was challenging to simultaneously manage my depression and my many worried superiors. I felt that at times I was not given the space to heal, despite being well connected to my own mental health team.”
But he recovers and ends with this comment:
“My family and program director recently told me how proud they were of me for going into the hospital. I think that is pretty freaking cool.”
A few thoughts:
- This is an excellent paper.
- Dr. Bullock is bold and raw.
- I think many will agree that the essay is pretty freaking cool – and published, no less, in NEJM.
The New England Journal of Medicine paper can be found here:
https://www.nejm.org/doi/full/10.1056/NEJMp1917203
Reading of the Week. Every week I pick articles and papers from the world of Psychiatry.
Recent Comments