From the Editor
Is he going to get sick again?
It’s a question that we often ask when a patient overcomes depression and happily leaves our office. For many patients, depression is a chronic illness – and so, remission is followed by relapse. Is it possible to predict patients with depression who are in remission but at risk of relapse?
Can we predict a future relapse – or is this an exercise in fortune-telling?
This week’s Reading is a paper from The American Journal of Psychiatry. Drawing on a long-term study, they look at the pattern of acute illness, remission, and relapse. Using statistical analyses, the authors seek to find a way of predicting relapse.
Spoiler alert: they do.
DG
Depression and Relapse
“A Brief Clinical Tool to Estimate Individual Patients’ Risk of Depressive Relapse Following Remission: Proof of Concept”
Lewis L. Judd, Pamela J. Schettler, A. John Rush
The American Journal of Psychiatry, 1 November 2016
http://ajp.psychiatryonline.org/doi/full/10.1176/appi.ajp.2016.15111462
The aim of depression treatment is sustained symptom remission and functional recovery. Full remission of all symptoms of a major depressive episode (as opposed to symptom improvement to a subsyndromal status) is far more likely to lead to a stable well period with good everyday functioning and a lower risk of depressive episode relapse. We previously reported that among 197 patients in the National Institute of Mental Health Collaborative Depression Study who achieved full remission from a major depressive episode, the rate of relapse was 16% over the next 6 months and 26% over 1 year. Others have also noted a modest but meaningful rate of relapse among depressed patients who have achieved complete remission.
We currently have no patient-level indicators with which to plan care for individual depressed patients who have reached remission. Current guidance recommends visits every 1 to 6 months based on clinical judgment. However, if we could develop a clinical tool for estimating the likelihood of relapse for a given patient after complete remission, we would be able to tailor the follow-up visit schedule individually. Patients more likely to relapse could be followed up more often, in person or by telephone, whereas those at lower risk of relapse could be seen less frequently. Care would be more efficient, and, if needed, interventions could be delivered in a more timely fashion to patients with impending or actual relapses.
Our aim in this study was to determine whether a limited number of symptoms could be combined to create a person-level metric for guiding clinical decision making with sufficient accuracy that it could be used to inform care planning for depressed patients who have achieved full remission. The Hopkins Symptom Checklist–90 (SCL-90) provides an ideal instrument for this purpose because it includes a wide range of mood, somatic, behavioral, and cognitive symptoms.
So begins a new paper published in The American Journal of Psychiatry.
Here’s what the authors did:
· They drew data from the National Institute for Mental Health Collaborative Study of Depression. That study looked at people seeking treatment in one of five U.S. centres between 1978 and 1981, with follow up stretching up to 31 years. People were white (for genetic purposes) and needed to speak English. The sample excluded people with bipolar, schizophrenia and schizoaffective disorder. As part of that study, extensive demographic information was collected, as well as follow up data, including clinical status on a weekly basis. Trained professional raters did follow up testing every six months for five years, then annually. The follow up included people doing SCL-90s (the Hopkins Symptom Checklist – a self-report checklist of 90 symptoms) with regularity.
· The study authors considered people who had been in remission for at least 8 weeks. The study authors then used mixed-model logistic regression to consider which symptoms on the SCL-90 were predictive of a relapse within six months. Further statistical analyses were done, finding 12 symptoms that were most linked to relapse.
· The study authors also considered the rate of relapse depending on the number of the 12 symptoms that were present.
Here’s what they found:
· There were 487 people in the National Institute for Mental Health Collaborative Study, after the exclusion criteria; 194 had met criteria for remission with 188 having full data. 73 had a depression relapse.
· Of the 188 people, most were female (58.5%), had some college (56.4%) and were married or living with a partner (56.4%). The mean age was 37.8.
· In terms of the depression experience: “About one third (34.0%) were in their first depressive episode at study intake, 43.6% had experienced one or two previous episodes, and the remaining 22.3% had three or more previous episodes.” The majority were inpatients at the time of intake (71.8%). !!
· Among the symptoms identified on SCL-90 connected with a relapse: “feeling blocked in getting things done,” “feeling inferior to others,” “trouble concentrating,” “worrying too much about things.”
· “We found that experiencing any one or more of the 12 symptoms most predictive of relapse at a moderate or worse level of severity in the past week resulted in a sensitivity of 80.8% for identifying relapse occurrences within the next 6 months and a specificity of 51.2% for identifying true nonrelapses…”
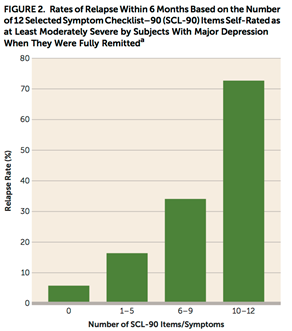
· Pulling this together: “A simple count of the number of symptoms (0–12) self-reported at a moderate or worse level of severity during the past week created a score that was highly related to the risk of relapse. A score of 0 was associated with a low (5.8%) risk for depressive relapse in the next 6 months, suggesting that these patients may be managed by, for example, telephone visits at 3 and 6 months. Patients with a score of 6–9 had a 34.1% risk of relapse, and those with a score of 10–12 had a 72.7% risk of relapse; for these patients, more frequent follow-up contacts would be warranted to intervene at the first sign of symptom worsening.” See graph:
They conclude:
In summary, about 1 in 7 fully remitted, formerly depressed patients experienced clinically meaningful depressive relapses over the next 6 months. These relapses were associated with a far worse course of depression over the ensuing 5 years. As a proof of concept, we have demonstrated that a brief 12-item symptom-based tool can provide an estimate of the risk of relapse for individual patients. Such simple, clinically based indicators can provide a platform onto which laboratory-based measures could be added to further personalize patient care.
The paper runs with an editorial by Dr. Robert M. A. Hirschfeld, which you can find here:
http://ajp.psychiatryonline.org/doi/full/10.1176/appi.ajp.2016.16080924
Robert M. A. Hirschfeld
He opens:
Depression is a recurrent illness, and all too often a chronic one. The recurrence and chronicity of depression were demonstrated in a series of reports from the National Institute of Mental Health Collaborative Depression Study (CDS), in which 431 patients with major depressive disorder were followed for nearly two decades. Most patients (70%) recovered within a year. However over a third (36%) relapsed within 12 months after their recovery. One in five of these patients continued to be depressed for 2 years, and the majority remained persistently depressed for at least 5 years. Patients had significant depressive symptoms nearly 60% of the time during 12 years of follow-up. Quality-of-life assessments over 10 years of follow-up depict substantial ongoing impairment and debility. The clinical course of depression is grim.
He makes a few points:
· He notes that there are “a variety of effective treatments…”
· But – “What the literature doesn’t tell us is how often to follow our patients with depression.”
· He summarizes the Judd et al. paper, noting that it “sheds light constructively on this important question…”
He goes on to argue that:
[T]he article does not recommend a specific score above which to increase vigilance. I would recommend that clinicians increase vigilance when three or more items are positive. This will identify over 60% of patients who will relapse and successfully screen out three-quarters of those who will not. My rationale is that the cost of a false positive is not that high.
He concludes: “A caveat is in order: The analyses supporting the creation of this clinical tool are exploratory, and replication is needed. This is well worth doing.”
A few thoughts:
1. This is a good study – it seeks to find ways of predicting relapse after remission
2. Given that many patients find that depression is a chronic if episodic illness, the study authors are looking at a practical issue.
3. They also have a practical finding: a dozen questions out of the SCL-90 – a self-administered test – are relevant. The study authors push further, seeing practical implications for treatment: “Such a person level indicator can be used to tailor the follow-up schedule for each remitted patient based on his or her individually identified risk of relapse and potentially to initiate interventions in a more timely fashion when needed.” Nice.
4. Like Dr. Hirschfeld, it’s easy to be enthusiastic about this paper – but a bit cautious, as well. The paper draws data from a sample that isn’t necessarily representative of many patients today. It also looks at relapse over just 6 months – making us hope for more work in this area.
5. As I have commented before, measurement-based care has great potential – not in terms of replacing the clinician, but in terms of better informing decisions (in this case, follow-up frequency).
Reading of the Week. Every week I pick articles and papers from the world of Psychiatry.




Recent Comments