From the Editor
He isn’t able to work. He often can’t get out of bed. His partner is beside herself. And his diabetic management is poor.
He’s the sort of patient who we see often – in specialist offices (like mine) and in family medicine clinics, and also in emergency departments and on hospital wards. His depression is affecting his life, his family, his workplace – and, yes, his health. Here’s a quick question: how much higher are his health-care costs than those who don’t struggle with depression?
In this week’s selection, we look at a new paper by Maria Chiu et al., considering the costs of depression and distress.
 Distress and depression: Painful to patients – and costly to the system?
Distress and depression: Painful to patients – and costly to the system?
In this Reading, we review the paper, and consider the larger context.
DG
Depression and Distress
“The direct healthcare costs associated with psychological distress and major depression: A population-based cohort study in Ontario, Canada”
Maria Chiu, Michael Lebenbaum, Joyce Cheng, Claire de Oliveira, Paul Kurdyak
PLOS ONE, 5 September 2017
http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0184268
Depression is an important public health concern that impacts approximately 350 million people worldwide and is the third leading cause of disability globally. In the United States, approximately 19.2% of adults experienced a major depressive episode at some point in their lives, while in Canada, the prevalence was 11.3%. In addition to people with major depressive disorder (MDD), there are individuals who exhibit psychological distress, a more prevalent nonspecific condition characterized by symptoms of depression, anxiety and related somatic symptoms. Psychological distress is associated with low socioeconomic status, unemployment, poor health and increased risk of mortality. Despite the increased health burden of depression, few population-based cohort studies have examined the costs associated with major depression and far fewer studies have examined costs related to psychological distress.
Previous costing studies for depression have focused on patients in primary care or psychiatric care settings rather than population-based samples, which may be more representative of all people with depression, particularly those who do not seek health services. Many studies have also estimated costs with limited adjustment for confounding factors, such as age, sex, income, lifestyle risk factors, and somatic illnesses. Moreover, previous studies examining the cost of psychological distress did not have an MDD group for cost comparison and often relied on self-reported healthcare utilization. Finally, there is insufficient evidence on which healthcare sectors are most associated with depression and psychological distress.
The primary objective of this study was therefore to determine the direct healthcare costs associated with psychological distress and major depression in Ontario. The secondary objectives were to understand how these costs vary by healthcare sector and what proportion of total costs were for mental health and addictions (MHA) versus non-MHA related healthcare services.
So begins a paper by Chiu et al.
Here’s what they did:
- To establish the study cohort group, the data was drawn from the Ontario sample of the Canadian Community Health Survey on Mental Health and Well Being, conducted by Statistics Canada in 2002. That data was linked to other health data (through people’s public health insurance).
- Exclusion criteria included diagnoses of schizophrenia and schizoaffective disorder, and hospitalizations for bipolar.
- Using a DSM-IV definition, people were in the depression group if they met criteria for a Major Depressive Episode in the past 12 months. People were included in the psychological distress group if they scored 8 or more out of 24 on the Kessler 6 scale, and weren’t in the depression group.
- Costs for hospitalizations, ED visits, and outpatient visits were captured within health administrative databases, and included for 11 years (to 31 March 2013).
- Statistical analyses included a two-part model: “where the first part models whether costs occurred using a probit model and the second part models the level of costs among those with non-zero costs, conditional on incurring costs using a generalized linear model with a gamma distribution and a log link.” Costs were calculated on a per capita basis, as well as population wide.
Here’s what they found:
- There were 9,965 individuals: 651 with psychological distress, 409 with MDD and 8,905 comparison group individuals.
- “The weighted prevalence of psychological distress and MDD was 6.6% and 3.9%, respectively.”
- Demographically: “Individuals with psychological distress and MDD were significantly younger than the comparison group (40.8 and 39.3 vs. 44.3 years, respectively) and were less likely to be married or in common-law relationships.”
- Per capita. “The annual per-capita total costs were similar between the psychological distress ($3,364) and MDD ($3,210) groups and both had higher costs than the comparison group ($2,629). The psychological distress and MDD groups incurred higher healthcare costs in all sectors examined (i.e. outpatient, ED, hospital and other healthcare sectors)…” In terms of mental health and addiction (MHA) vs. non MHA costs: “Although MHA costs were lower in the psychological distress group relative to the MDD group, they incurred greater non-MHA costs than the MDD group…” With regard to MHA costs: “only 4% of the costs incurred by those with psychological distress are associated with MHA-related health services compared to 14% among individuals with depression.”
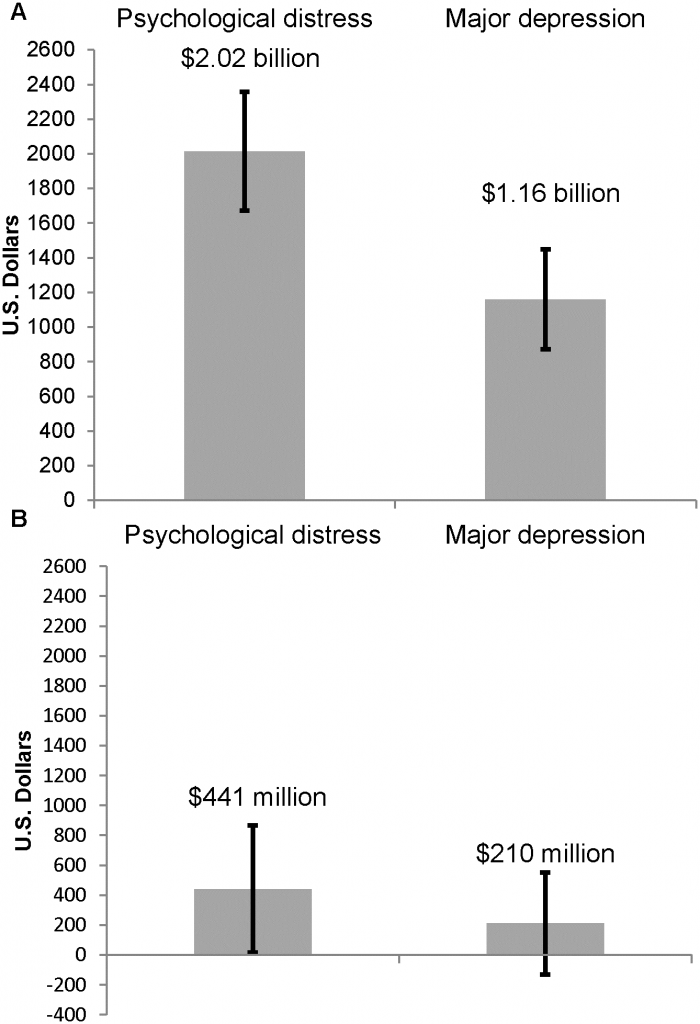
- Population wide. “The age-and-sex adjusted annual absolute healthcare costs were $2.0 billion for the psychologically distressed population and $1.2 billion for the MDD population.” See figure below.
They go on to conclude:
In this population-based study, we found that people with psychological distress and major depression incurred similar per-capita direct healthcare costs and these costs were greater than those without either condition. These two groups differed in the way the totals were reached, with depressed individuals incurring higher mental health and addiction-related costs and psychologically distressed individuals incurring higher non-mental health and addiction costs.
A few thoughts:
- This is a good paper.
- It’s not surprising that depression was associated with higher health-care costs – but so was distress. And that’s a finding similar to an American study (Katon et al.).
- The paper has strengths, including that Chiu et al. tapped big databases (possible because of Ontario’s public health care system) – though it should also be noted that health costs didn’t include drug costs (because Ontario’s public health care system largely doesn’t cover such costs for the non-elderly).
- What now? The paper shows significantly higher costs for people with depression and distress. Yet it’s also true that the type of targeted, evidence-based therapies that would help such people (think cognitive behavioural therapy) are generally not available in Canada. To the patient who is stressed out and thus less likely to regularly take his diabetic medications, available CBT would be difficult to find, even in a big city (and nearly impossible in a rural area). Looking at British Columbians, Puyat et al. found just 13% of people with depression had CBT or other forms of “minimally adequate counseling/psychotherapy.”
- Public coverage for CBT and other evidenced-based therapies is increasingly discussed in Canada. In August, the Ontario Health Technology Advisory Committee (OHTAC) released a draft report on “Psychotherapy for Major Depressive Disorder and Generalized Anxiety Disorder.” Such a report of a committee of an arms-length government body may not seem particularly exciting, but Health Quality Ontario holds sway with the Ontario government. And that province has already committed itself to more CBT funding. Other provinces are eyeing these changes, too. (Manitoba now covers CBT for first responders.) The summary of the OHTAC report can be found here: http://www.hqontario.ca/Portals/0/Documents/evidence/open-comment/recommendation-psychotherapy-1708-en.pdf. In the Toronto Star, Alex Munter, CEO of Children’s Hospital of Eastern Ontario, endorsed the report, writing: “An Ontario government agency has floated a game-changing idea that could put life-saving mental health treatment within reach for many who desperately need it.” You can find his article here: https://www.thestar.com/opinion/commentary/2017/09/09/put-critical-mental-health-care-within-reach-of-all.html. And I also put the pen to paper. My submission to the committee can be found here: http://davidgratzer.com/blogging/public-coverage-for-evidenced-therapies-for-depression-and-anxiety/.
Reading of the Week. Every week I pick articles and papers from the world of Psychiatry.


Recent Comments