You can’t change what you can’t measure.
So suggests Dr. David Goldbloom, Chair of the Mental Health Commission of Canada, on the release of the Commission’s new report.
Reports from government and government agencies aren’t exactly uncommon in health care. Too often, they are heavy in rhetoric and light in impact. Last Thursday, the Commission released: Informing the Future: Mental Health Indicators for Canada. This report is different; it’s worth careful consideration. The Commission’s work offers the first national-level set of indicators to identify and report on Canadians’ mental health. This report considers 13 indicators; in April, a fuller report will contain 63 indicators.
Here’s the link:
http://www.mentalhealthcommission.ca/English/informing-future-mental-health-indicators-canada
(Because of firewall and browser issues, I’ve also attached the PDF.)
Dr. David Goldbloom
Informing the Future has already gained much media attention. The Toronto Star, for example, ran two articles. No wonder: this project is both important and timely. We as a society are discussing more and more the mental health needs of Canadians (a very appropriate comment to make just after Let’s Talk Day). But, at the same time, there remains a general lack of information, especially compared to other areas of medicine. We know 5-year cancer outcomes for people with breast carcinoma in, say, Calgary, but what do we know about depression recovery in Montreal?
Very basic questions could be asked. How does mental illness affect Canada’s workforce? How well do we serve the needs of those with mental illness?
Of course, many have studied such issues, including Statistics Canada. Quickly and graphically, the Mental Health Commission’s report pulls together information, and runs through 13 indicators – providing the data (good) but also providing context in a simple red-yellow-green scale and with sensible commentary (very good). The indicators are intelligently picked and relevant. The report is likely to have a significant impact in the coming years.
Consider suicide. The report states that “Suicide is arguably the most tragic consequence of mental illness.” Drawing on Statistics Canada data, the report notes 10.8 suicides per 100,000 population, higher than some G8 nations. More concerning: the rate hasn’t dropped over the past decade. The Commission gives this indicator a red, indicating “significant” concern.
Another indicator is mental-illness-related disability claims under the “focus” of Economic Prosperity.
The Commission looks at CPP-disability claims, drawing on Service Canada data.
I reproduce the graphic from page 15 of the report (thanks to the Commission’s Glenn Johnson):
Of all claims, 30.4% are for mental health reasons, significantly up from 2004. “Mental disorders are the largest diagnostic class when compared to disability benefits for other health reasons.”
So, to summarize:
· Nearly a third of all people on CPP Disability qualified because of mental illness. (!)
· The percentage of mental-health claimants has soared since 2004. (!!)
Speaking to the latter point, the report questions as to whether this rising percentage represents more mental illness in society or a reduction in stigma (meaning that people are willing to make a mental illness-related claim).
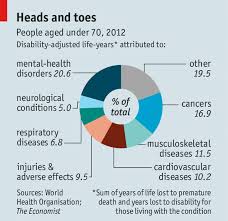
Though other indicators are important, this one strikes me as particularly important, since it lays to waste the usual assumptions that mental illness isn’t particularly common or disabling. In fact, it’s both. British economist Richard Layard has made a similar argument in the United Kingdom and draws on WHO data (from Western Europe). He observes that mental illness is a more common reason for lost years due to disability for working-aged people than neurological conditions, respiratory diseases and injuries – all put together.
This graph summarizes his findings:
Source: The Economist
Layard’s work – like the Commission’s – suggests that our problems with mental illness aren’t simply tragic and unfortunate, but also economically significant.
Where do we go from here? The Mental Health Commission of Canada has released several relevant reports and they are all online, including one on suicide prevention.
Along these lines, Drs. Paul Kurdyak and Sanjeev Sockalingam, both psychiatrists, argue for better screening and triaging of mental illness. In a recently published Ottawa Citizen op ed, they go further, praising the work of the Mental Health Commission and advocating for much more. They champion a performance measurement system focused on patient outcomes. And though that undertaking would be great, they note the incredible need:
[S]hockingly, only one in three patients discharged from a psychiatric hospitalization sees a primary care physician or psychiatrist within a month in Ontario, as reported by Health Quality Ontario. This poor post-discharge follow-up rate is far worse than the nearly 100 per cent of patients who see a physician following a hospitalization for heart failure.
Provocative.
Further reading? Find the Kurdyak and Sockalingam op ed here: http://ottawacitizen.com/news/national/kurdyak-and-sockalingam-how-canada-fails-people-with-mental-illnesses
The Toronto Star articles on Improving the Future can be found here:
http://www.thestar.com/news/canada/2015/01/22/8-key-numbers-in-canadas-mental-health-report.html
and
http://www.thestar.com/news/canada/2015/01/22/mental-health-report-warns-of-caregiver-stress-suicide-rates.html
Reading of the Week. Every week I pick a reading — often an article or a paper — from the world of Psychiatry.


Recent Comments