From the Editor
“To say that I didn’t know my great-uncle, Wolfe Levine, would understate things. I didn’t even know of such an uncle, brother of my mother’s father (a grandfather with whom I was close). In retrospect, it’s clear that my great-uncle was simply unmentionable.”
So begins Howard Husock, Vice President of the Manhattan Institute for Public Policy, in a long essay that traces the illness and institutionalization of his great uncle.
The piece asks a simple question: “Are we treating the mentally ill better today than we did a century ago?”
It’s a beautiful essay, that touches on history, psychiatry, and a family member who was “unmentionable.”
DG
Illness and Society
“Dreams of My Uncle”
Howard Husock, City Journal, Spring 2017
https://www.city-journal.org/html/dreams-my-uncle-15124.html
To say that I didn’t know my great-uncle, Wolfe Levine, would understate things. I didn’t even know of such an uncle, brother of my mother’s father (a grandfather with whom I was close). In retrospect, it’s clear that my great-uncle was simply unmentionable. His story would have been profoundly embarrassing for my grandparents, the first in their immigrant families to join the middle class. We’d write it off now to what we call the stigma of mental illness.
Wolfe Levine’s life story is tragic, dating from an era of large, public mental health institutions that we have sought to put behind us. His journey to the Lima State Hospital for the Criminally Insane in Lima, Ohio, began in 1910 with a criminal conviction: a one-to-five-year sentence in the Ohio State Reformatory in Mansfield for pickpocketing. It was just six years after Wolfe had immigrated to America, at 14. Theft was not a shocking charge against someone who lived in Cleveland with his widowed, single mother and her three other children on a Scovill Avenue block of ramshackle frame houses, along with other Russian Jewish families, near the heart of that community around East 55th Street. Wolfe’s occupations had included “newsboy” and laborer. After his pickpocketing conviction, he would never again be a free man.
State records show that, after less than two years in the state reformatory, Wolfe exhibited “persecutory delusions” and “auditory hallucinations” and was at times “catatonic.”
So opens an essay by Howard Husock from the spring issue of City Journal.
The piece describes the life of his great uncle. After conviction for a minor crime, Levine begins a journey from institution to institution to institution. He starts in the Ohio State Reformatory; he is transferred to the Lima State Hospital for the Criminally Insane; he is then transferred again, to the Columbus State Hospital, and again, to the Tiffin State Hospital – until it closes; finally, he comes full circle, returning to the Lima State Hospital. Levine lives in many institutions – and there are many years of living in institutions. As Husock notes: “He would die in state-hospital custody in 1982, at 92, having spent 72 years in institutions. In the language of latter-day reformers, he had been ‘warehoused’ for his entire adult life.”
The essay also considers the care (or “warehousing”) of those with mental illness in the United States – though if Levine had emigrated from Russia to Toronto instead of Cleveland, his experience would likely have been similar.
Over Levine’s long life, North America has seen institutionalization and deinstitutionalization.
Husock reviews the history:
- Drawing from Rutgers historian Gerald Grob’s work, Husock notes that the laws of the time “posed no serious obstacle to commitment…” with legal procedures “administered in a loose and informal manner.” Levine is convicted of pickpocketing, and is never free again.
- Husock notes that many were institutionalized in the early twentieth century; by 1940, some 450,000 Americans were in state psychiatric hospitals. Lima State Hospital – where Levine lives, leaves and then returns to – “boasted 17 wings for 1,400 patients and was considered the largest poured-concrete structure in the world prior to the construction of the Pentagon.”
- Of course, such large institutions existed across the United States. (In Canada: the Queen Street Asylum was once the tallest non-military building in this country.) They were filled with people – and death. Citing a British statistician who looked at nineteenth century institutions, Husock writes: “Of every hundred cases, 34 percent would recover by the end of one year, 29 percent would die, and 36 percent would remain at the stationary level.”
- Public enthusiasm for state psychiatric facilities soured, and deinstitutionalization began in the 1960s. By 2015, the number in state psychiatric facilities had fallen to 45,000.
- What happened to the chronically mentally ill? “The Bureau of Justice Statistics has estimated that 365,000 adults with serious mental illnesses are behind bars, and an additional 770,000 are on probation or parole.” So, they are in the prison system – and in our streets. “The Department of Housing and Urban Development estimates that, of some 564,000 homeless individuals identified on a single day in January 2015, some 25 percent – 140,000 – were seriously mentally ill.”
He closes by drawing on Meyer:
It’s worth rediscovering the sentiment expressed by Adolph Meyer, a physician on the staff of the Kankakee (Illinois) state asylum, in 1893. Meyer believed that the state had an obligation to provide every insane person with “the benefit of treatment and supervision by a competent physician.” We might argue about whether those who can afford such treatment on their own, or whose families can afford to help them, should receive public assistance. But leaving Wolfe Levine’s successors on the street or in isolation behind bars suggests that – in practice, at least – we have become not more but less compassionate about the severely mentally ill.
A few thoughts:
- This is a good essay, personal – yet rich in detail and steeped in history.
- It’s difficult not to feel the deep tragedy of this story. Before proper medications, many of those with mental illness simply ended up in the asylum system or in the jail system.
- The author asks a provocative question: “Are we treating the mentally ill better today than we did a century ago?” Later in the essay, as he considers the high number of mentally ill who are homeless, he clearly wonders if we are.
- From a treatment perspective, the world is so different today than when young Wolfe Levine began to experience hallucinations (roughly eleven decades ago). Now there are antipsychotics and evidence-based therapies. I think of Levine in jail, sick with hallucinations. And then I think of a young man who recently entered my hospital’s Psychiatric Intensive Care Unit convinced that his neighbours were trying to poison him; ten days after the admission, my patient left, free of his paranoia, primarily due to the benefit of medications.
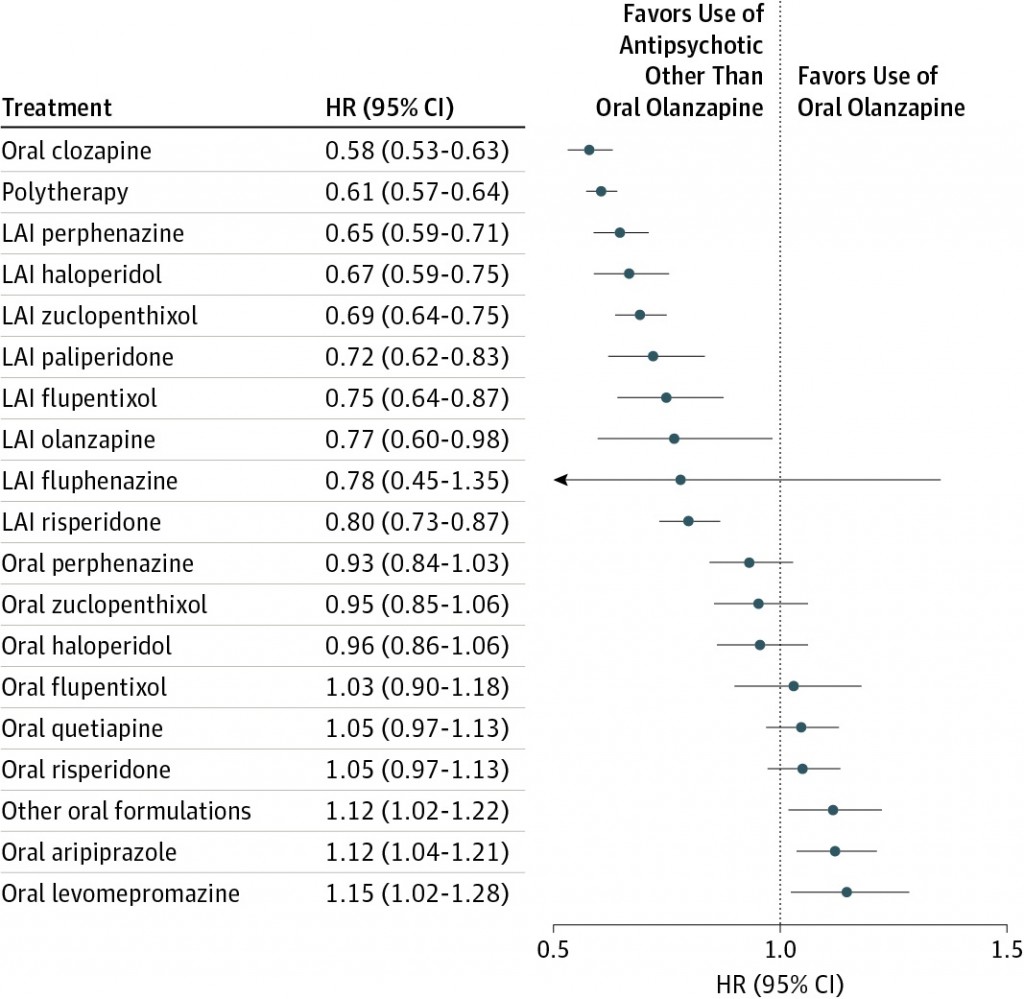
(As a side note: that’s not quite to say that new medications are better. I note the new JAMA Psychiatry paper showing the superiority of older depot medications and clozapine to new oral antipsychotics.
Still, compared to the straightjackets and the opiate sedatives offered to people like Levine at the time of his psychotic break, our medication options are infinitely superior.)
- But is the world so different in terms of outcomes? Those with severe, persistent mental illness live far fewer years than the general population; a World Psychiatry paper found a greater reduction in life expectancy for those with severe mental illness than for those who smoke. And there is evidence that the mortality gap between the general population and those with schizophrenia is growing (as Nielsen et al. found by looking at Danish data from 1980 to 2010). Husock writes of the United States and homelessness, but the statistics are similar north of the 49th parallel. Levine ended up in the jail system. So do many of our patients today.
- It’s easy to see how Husock – and others – can be nostalgic for the asylums of old; that is, as they describe it, “a protected place where safety, sanctuary, and long-term care for the mentally ill would be provided” (Husock quoting from the Sisti et al. paper). Of course, nostalgia has its limits. As CAMH CEO Catherine Zahn blogged in response to that paper, “surely, we can do better than return to a 19th century solution.” (You can find her full comments here: http://camhblog.com/2015/02/21/never-goin-back/.)
- I’ll close on a positive note. Though stigma still exists, people like Husock’s great uncle are no longer unmentionable.
Reading of the Week. Every week I pick articles and papers from the world of Psychiatry.



Recent Comments