From the Editor
I spent a dozen years working at a community hospital. One of my richest experiences was working with cancer patients and their families. For so many patients, not surprisingly, cancer isn’t just a physical illness, but a psychiatric one, too – patients often experience depression and anxiety.
How common is PTSD in cancer patients? Surprisingly little work has been done in the area. In this week’s Reading, we look at a new study that considers PTSD and cancer. The study is particularly impressive in that patients were followed for years after diagnosis.
 Big diagnosis, big treatment, big psychiatric problems?
Big diagnosis, big treatment, big psychiatric problems?
In this Reading, we consider the paper and its findings.
And, with an eye on treatment for those with or without cancer, we consider a good news story: on Sunday, the Quebec government committed itself to cover psychotherapy for those with depression and anxiety in the public system.
DG
Cancer and Mental Health
“Course and predictors of post-traumatic stress disorder in a cohort of psychologically distressed patients with cancer: A 4-year follow-up study”
Caryn Mei Hsien Chan, Chong Guan Ng, Nur Aishah Taib, Lei Hum Wee, Edward Krupat, Fremonta Meyer
Cancer, 20 November 2017 Early View
http://onlinelibrary.wiley.com/doi/10.1002/cncr.30980/full
Depression and anxiety are known to be prevalent in patients with cancer, but rates of post-traumatic stress disorder (PTSD) have been examined less frequently in this population. Despite the identification of cancer as a potential trauma in the fourth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV), PTSD in patients with cancer remains a relatively new field of research.
Cancer diagnosis and treatment are unique, long-term traumatic stressors, as first described by PTSD field trials for the DSM-IV. The concept of cancer as an enduring risk is important given the potential for disease relapse and progression. PTSD is an especially pertinent issue in cancer given its association with maladaptive patterns of avoidance behavior, which may increase the likelihood of nonadherence with cancer surveillance or treatment and poorer cancer outcomes.
There is limited knowledge about how the rates of PTSD and other psychiatric disorders among patients with cancer may differ according to nation, region, and culture. Findings from the BQUAL study, which focused on symptoms of PTSD among oncology patients up to 6 months after their initial cancer diagnosis, suggest that Asian patients with cancer may be at greater risk of PTSD symptoms compared with patients of Caucasian descent.
Worldwide, studies of PTSD in patients with cancer have reported incidence rates ranging from 0% to 6% when diagnostic structured clinical interviews are used. Only 6 existing studies of 100 or more patients, mainly conducted among women with breast and gynecologic cancers but also among bone marrow transplantation recipients (range, 102-506 patients), have reported the prevalence of PTSD using a validated diagnostic interview. Of those studies, only Voigt et al examined PTSD with a longitudinal design using repeated clinical assessments over the course of 1 year and observed that more than one-half of patients displayed 1 or more PTSD symptoms at 1 year after the cancer diagnosis.
To the best of our knowledge, there are no studies examining PTSD in patients with cancer that have used gold-standard clinical interviews and followed a cohort for a period as long as 4 years. The objective of our current study was to assess the course and predictors of PTSD in adult patients with cancer over a 4-year period in a South-East Asian population. We hypothesized that the presence of psychological distress at diagnosis and after treatment would predict PTSD, and that PTSD would persist in the long term for a small proportion of the sample.
 Caryn Mei Hsien Chan
Caryn Mei Hsien Chan
Here’s what they did:
- The study was run out of an academic centre in Malaysia.
- A month after diagnosis, patients had an interview. If they were eligible for the study and consented, they were screened for psychological distress (Hospital Anxiety and Depression Scale total cutoff score ≥16). The distressed were then given the PTSD module of the Structured Clinical Interview for the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (SCID) at 6 months and at 4 years.
- Inclusion criteria included any form of cancer. Exclusion criteria included those who were too ill to be interviewed.
- Statistical analyses were done, including separate binary logistic regression to test for predictors of PTSD at 6-months and 4-years follow-up.
Here’s what they found:
- Of the 469 people referred, 439 individuals did the appropriate scales and interviews. At the 6-month follow-up, 203 of 222 had elevated HADS scores – and thus underwent the structured clinical interviews. 210 deaths occurred in the study period; of the 247 of those remaining, 245 were re-interviewed.
- Demographically: participants were female more than male, older (55-69), and had secondary education or more. In terms of demographics, the authors note: “patients did not appear to differ from each other significantly.” In terms of cancer, most had breast, GI, or lung cancers, though various cancers were studied; patients tended to have later stage cancers (the majority with PTSD and subsyndromal PTSD had stage IV cancers).
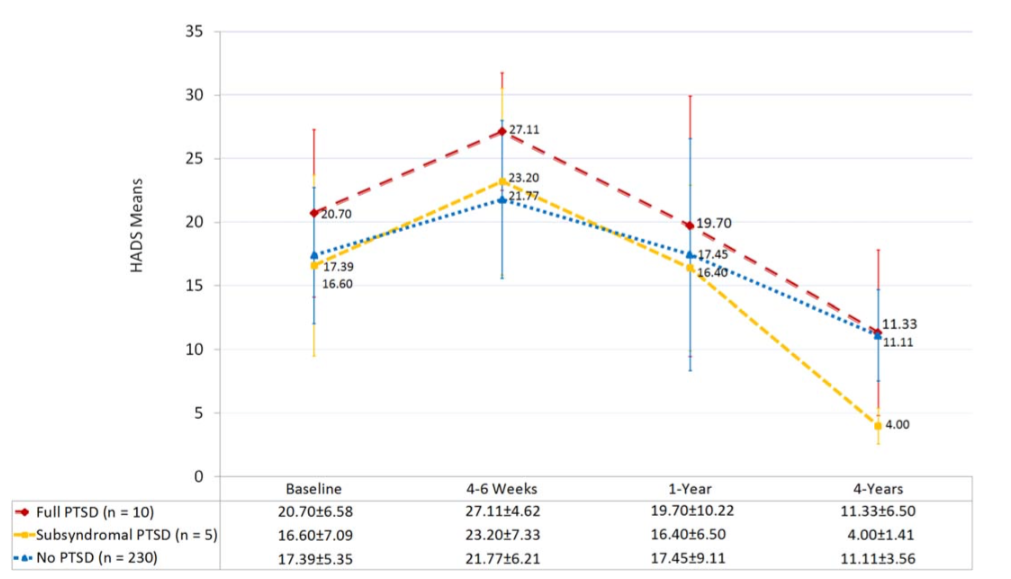
- “At the 6-month follow-up, 27 of 203 patients (13.3%) met the full criteria for PTSD, and another 17 patients (8.4%) had subsyndromal PTSD symptoms. This yielded a 21.7% PTSD incidence when patients with both full and subsyndromal PTSD were aggregated.”
- “At the 4-year follow-up, 10 of 245 patients (4.1%) had full PTSD, and 5 (2%) had subsyndromal PTSD. When patients with both full and subsyndromal PTSD were combined, this yielded a 6.1% incidence.” See figure below.
- In terms of different cancers: “Inspection of the differences at the multivariate level using logistic regression analyses revealed that patients with breast cancer were 3.68 times less likely to develop PTSD by the 6-month follow-up assessment…”
This study is the first in this region to examine PTSD longitudinally at 2 different times, providing data that span a full 4 years using gold-standard clinical interviews. Our findings add to the literature on PTSD among patients with cancer, because many of the previous studies are mainly conducted by self-assessment and remain largely cross-sectional. To our knowledge, this study represents 1 of the longest follow-up studies to date examining the course and predictors of PTSD among patients with cancer.
It is striking to note the high rate of PTSD in this study.
A few thoughts:
- This is a good study.
- There is much to like here, including the long follow-up period. I note also the use of structured interviews for diagnosis.
- It’s important to note that the authors looked at PTSD but also subthreshold PTSD. (Some of the media reports, incidentally, didn’t appreciate the distinction.) It’s very true that the rate of PTSD was high at 6 months. That’s less true at 4 years (6.8% of the US population has PTSD – but that may be an apples-to-oranges comparison since this study didn’t involve Americans).
- This study covers patients in Asia. Would North American results have looked different? I’m not speaking to study design, but rather cultural acceptance (or lack of acceptance) of different cancers in different places, and the possible implications to PTSD.
The authors, for the record, did consider cultural acceptance of difference cancers. For example, breast cancer: “Breast cancer appeared to be a protective factor for PTSD at 6-months, but not at 4-years, follow-up. Because breast cancer is a very common malignancy, it is possible that greater societal understanding and the wider availability of support programs tailored for breast cancer (compared with the fewer support programs for patients with other cancer types) initially serve as protective factors against PTSD, but that this protective effect attenuates with distance from the original diagnosis.”
- In his blog, CBC’s Brian Goldman, a Toronto physician, offers a Canadian perspective on the study: “In the past, cancer treatment was all about fighting the cancer. Now, two out of every three people who are diagnosed with cancer are expected to live at least five years following the diagnosis. Canada has close to a million people living with cancer, a number expected to grow dramatically in the years to come. We’re going to need a lot more resources devoted to helping cancer survivors deal with the emotional fallout.”
Quebec and Therapy
“Psychotherapy: Quebec to invest $35 million in mental health”
Charlie Fidelman
Montreal Gazette, 3 December 2017
In Quebec, as in other provinces, psychotherapy services are not part of publicly insured health-care services although psychotherapy is a recognized treatment option for common mental disorders.
Inspired by a similar program in place in the United Kingdom for a decade, Quebec’s investment aims to establish the service, develop a reference framework, upgrade training of health professionals as well as set up a registry of recognized psychotherapists.
The article notes:
- A 2012 report for the Commissioner of Health and Welfare had called for the government to provide psychotherapy, estimating that coverage would save money by improving public health.
- In 2013, the Institut de la statistique du Quebec study estimated that more than 200,000 people had needed a consult for therapy, but couldn’t get it because they lacked insurance or the ability to pay.
The government announcement seems light in details except that the program will begin in 2018 and be available for those with depression and anxiety.
A few thoughts:
- This is a big announcement.
- The Ontario government has made a similar – if smaller – commitment in recent months.
- With details to be worked out in both provinces, much remains to be seen. That said, this much is clear: in the coming months, more and more people will have access to the therapy they need.
- Of course, there is much work to be done. Consider: more than a half million people in the UK (England) completed publicly-covered psychotherapy last year, with 51% moving to recovery.
Reading of the Week. Every week I pick articles and papers from the world of Psychiatry.
Recent Comments