From the Editor
For the patient sitting in front of you, depression is a weight around her shoulders, the reason she can’t enjoy her favourite activities or laugh at her partner’s jokes. Such is the patient experience.
This week, we have three selections, and all consider different aspects of this illness. In the first, we look at a paper from The Canadian Journal of Psychiatry. Julie-Anne Tanner (University of Toronto) and her co-authors draw on data to estimate the economic burden of depression in Manitoba. They conclude: “Depression contributes significantly to health burden and per patient costs in Manitoba, Canada. Extrapolation of the results to the entire Canadian health-care system projects an excess of $12 billion annually in health system spending.”

Manitoba: big prairie & big burden of depression
In the second selection, we review a short JAMA paper by Dr. Mark Zimmerman (Brown University) considering depression management. He recommends the use of the PHQ-9 in screening. As for treatment, he writes: “the PHQ-9 should be administered at each visit to quantitatively measure a patient’s treatment response.”
And in the third selection, returning to the patient experience, Dr. Carrie Bernard (University of Toronto) writes in CMAJ about her journey. “I am a committed family physician, skilled researcher and respected leader at my university. And I suffer from depression. Why is that so difficult to write?”
DG
Selection 1: “Economic Burden of Depression and Associated Resource Use in Manitoba, Canada”
Julie-Anne Tanner, Jennifer Hensel, Paige E. Davies, Lisa C. Brown, Bryan M. Dechairo, Benoit H. Mulsant
The Canadian Journal of Psychiatry, 13 December 2019
![]()
Mental illness and addictions are a significant burden in Canada, exceeding that of other chronic illnesses such as cancer and infectious disease.This extensive health burden results in greater use of health-care resources and a substantial economic burden, estimated to be as large as $51 billion in Canada in 2003. In Ontario, Canada’s most populous province, high-cost mental health patients were found to incur 60% higher average health care costs than other high-cost patients who had no mental health–related costs…
Because of its high incidence, chronicity, and associated morbidity, depression exerts the greatest burden of all mental illnesses: It is a leading cause of disability and excess mortality in Canada. In addition to its psychological symptoms, depression is associated with chronic comorbidities including diabetes, heart disease, arthritis, asthma, back pain, chronic bronchitis, hypertension, and migraines…
While several studies have assessed the economic burden of mental illness overall, few studies have focused on the per patient cost of depression in Canada.
So begins a new paper by Tanner et al.
Here’s what they did:
- They drew data from Manitoba databases for the study period of January 1, 1996, through December 31, 2016.
- Patients were assigned to the depression cohort based on diagnoses (recorded in hospitalizations and outpatient physician claims), as well as antidepressant prescriptions (based on drug claims).
- A comparison cohort of non-depressed subjects, matched for several things, including age, gender, and place of residence (urban vs. rural).
Here’s what they found:
- A total of 190,065 patients were included in the depression cohort and 378,177 patients in the non-depression cohort.
- Demographics: the mean age was 45 and people tended to live in urban areas (63.2% of depression cohort vs. 63.7% of non-depression cohort).
- “The number of patients who had any hospitalization during the study period was 50% higher in the depressed compared to the non-depression cohort (61.8% vs. 41.2%)… Depressed patients spent a mean of 8.3 days per year in the hospital compared to 1.9 days per year for non-depressed patients.”
- “While the vast majority of patients in both cohorts had a physician visit during the study period, more depressed patients had at least one family doctor (99.6% vs. 96.3%), specialty (97.1% vs. 89.6%), or physician psychotherapy (79.3% vs. 38.3%) visit compared to non-depressed patients.”
- “The mean direct medical costs associated with depression were more than 3.5 times higher than that of the non-depression cohort ($10,064 vs. $2,832 per patient per year)…” Social services costs were higher, too. See the figure below.
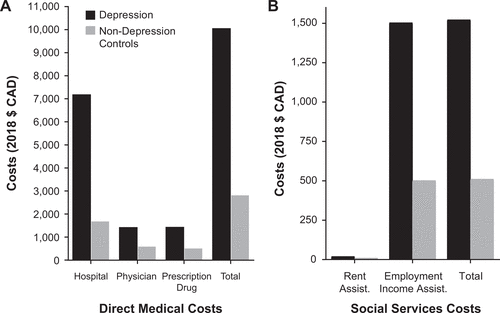
They conclude:
Based on our data, we project that each year depression costs the province of Manitoba and Canada an additional $400 million and $12 billion, respectively.
This is a good and important study, attaching an economic cost to the illness. That isn’t the way clinicians and patients typically think about depression.
The estimate is not without limitations, of course. The narrow definition of depression (at least one hospitalization, or five physician visits for depression, or one physician visit plus seven or more prescriptions for antidepressants in 2 consecutive years) would limit diagnoses to more severe cases. And the analysis of social services costs doesn’t consider forensic populations (the way, as an example, UK economist Richard Layard’s work on the burden of mental illness does). The point: this estimate is likely low.
Still, the number is relevant, and puts the illness experience in a larger, economic perspective.
https://journals.sagepub.com/doi/full/10.1177/0706743719895342
Selection 2: “Using the 9-Item Patient Health Questionnaire to Screen for and Monitor Depression”
Mark Zimmerman
JAMA, 18 October 2019

Clinically significant depression is one of the most common disorders presenting in primary care. It is a frequent comorbid condition in patients who have a variety of medical illnesses. Depression is associated with impairments in major role function and premature mortality and is common, with a yearly prevalence of 8% and lifetime prevalence of 19%. Because of its relatively high prevalence and associated psychosocial morbidity, depression is one of the most disabling of all medical illnesses.
Concerns about the under-recognition of depression in medical practice, particularly primary care, have led to calls for improved detection. The use of self-administered questionnaires to screen for depression has been recommended by several medical societies and organizations, although this has not been without controversy.
So opens a short paper by Dr. Zimmerman.
He continues by talking about the numerous scales available. “Many scales have been developed to assess depression. In clinical practice, self-report questionnaires may be preferable to clinician-rated scales because they require less professional involvement for administration.”
Dr. Zimmerman writes about the PHQ-9 – the “most frequently studied screening measure for depression in primary care…”
Screening
“The PHQ-9 was intended to be used as a screening instrument; it is not to be used to make a diagnosis of depression. Because it is a screening measure, a broad net needs to be cast and the threshold set lower to enhance the sensitivity of the measure.”
Balancing specificity and sensitivity: “the most frequently recommended cutoff on the PHQ-9 for a positive screen is a score of 10.”
Monitoring Outcome
“The PHQ-9 is a valid measure of symptom change. When measuring treatment outcomes in clinical practice, the magnitude of change in depressive symptoms is as great on the PHQ-9 as it is on clinician-based rating scales. In a primary care clinical trial, the use of a measurement-based care approach to treating depression with the PHQ-9, compared with treatment as usual, resulted in a significantly higher response rate (67.0% vs 59.7%) and remission rate (46.7% vs 42.8%) for depression.”
Severity Categorization
“Treatment guidelines for depression suggest that severity should be considered when selecting a treatment. The American Psychiatric Association guidelines for the treatment of major depressive disorder recommended either psychotherapy or pharmacotherapy as monotherapies for mild and moderate depression, and pharmacotherapy as the treatment of choice for patients with severe depression.”
But he notes that the PHQ-9 overdiagnoses severe depression and underdiagnoses mild depression. (!) With that in mind: “its use could result in fewer psychotherapy referrals and greater reliance on medication as a first-line treatment option.”
He concludes:
For patients being treated for depression, the PHQ-9 should be administered at each visit to quantitatively measure a patient’s treatment response. The type of depression treatment should only be determined by a clinician and not the PHQ-9 because it overclassifies depression severity.
This short paper is practical, as is his central recommendation: use of a scale that patients can do on their own (perhaps while in the waiting room). Dr. Zimmerman doesn’t comment on inpatient care, but the central recommendation – the use of the PHQ-9 – seems reasonable, perhaps at the beginning and end of hospitalizations.
Of course, a PHQ-9 is not perfect. For patients who may be overstating or understating their symptoms, this scale will yield a flawed result. But is that a serious criticism? All data, after all, should be put into a larger clinical perspective.
https://jamanetwork.com/journals/jama/fullarticle/2753532
Selection 3: “Disclosure”
Carrie Bernard
CMAJ, February 2020

I am a committed family physician, skilled researcher and respected leader at my university. And I suffer from depression. Why is that so difficult to write?
Apparently, I am not alone. According to the recent CMA National Physician Health Survey, 33% of physician respondents screened positive for depression and some are sharing their stories. Many of the physicians who discuss their mental health journeys, however, do so through the rearview mirror. Disclosure seems to happen mostly after the fact, when people have successfully navigated a path toward healing. The reasons for this are self-evident: stigma, fear of reprisals from regulators, and the challenge of speaking eloquently when all of one’s energy needs to be directed toward just getting through the day. It makes sense. But is this really the best way? I think that earlier disclosure can have benefits, ones I discovered on my own journey.
She talks about the loss of her mother to cancer, and taking a short period off work.
“By the time I went back to work at the university, being too busy seemed like a welcome reprieve from my emotional turmoil. I threw myself ever more deeply into work, leaving little time for exercise or rest. My anxiety did not abate with this fervent pace, and my mood started to slip. I started to avoid social situations because I felt disconnected from friends and colleagues. Instead of enjoying stories about others’ lives, I started to feel agitated and unable to listen, even to close friends.”
She opted for treatment.
“I started the medications, and the fog began to lift. Slowly, I started to cut back on work. I left some committees, took on fewer students and asked others to help lead projects. The one thing I didn’t do was disclose.”
She explains: “Telling my colleagues and superiors that I had been suffering from depression seemed to be a burden: would they then have to weigh and consider each and every request they made of me? This was too much to ask. So I kept things mostly to myself and I continued to muddle my way through.”
Over time, she concludes that disclosure is important, as is better balance in her life. “My disclosure allowed others to support me. It also helped me to feel a part of something bigger, even when I couldn’t contribute in the way I had in the past. This feeling was integral to my path back toward joy.”
She concludes:
Here’s what I have learned: we, as a medical community, must open the wellness discussions to include conversations about mental illness as it happens – in real time – so that those who suffer do not fear the repercussions of disclosure when they already have so much to bear. Disclosure, paired with the support of a caring medical community, can help ensure that everyone can remain a vital part of our team, even through illness, no matter what the source.
This is a lovely and important paper.
https://www.cmaj.ca/content/191/43/E1196
Reading of the Week. Every week I pick articles and papers from the world of Psychiatry.
Recent Comments