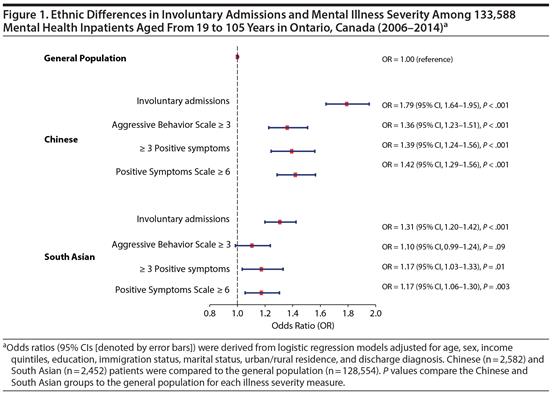
From the Editor
Younger and sicker.
This week, we look at a new paper published in The Journal of Clinical Psychiatry considering ethnicity and hospitalizations. Drawing on Ontario data, researchers looked at psychiatric hospitalizations for people of Chinese and South Asian descent, finding that they were younger and more ill at the time of admission.
 Hospitalizations, ethnicity… and access
Hospitalizations, ethnicity… and access
Lead author Maria Chiu of the Institute for Clinical Evaluative Sciences told the Toronto Star:
Cultural factors play a big role in these findings. While Asian people tend to have stronger family support, they are also faced with a higher level of stigma and it prevents people from seeking help early. Families may try to cope and keep the illness within the family until there is no choice but to go to hospital.
This paper is well designed. It’s also important, speaking to larger issues about access, stigma, and ethnicity.
DG
Ethnicity and Presentation
“Ethnic Differences in Mental Illness Severity: A Population-Based Study of Chinese and South Asian Patients in Ontario, Canada”
Maria Chiu, Michael Lebenbaum, Alice M. Newman, Juveria Zaheer, and Paul Kurdyak
The Journal of Clinical Psychiatry, 2 August 2016 Online First
https://www.psychiatrist.com/JCP/article/Pages/2016/aheadofprint/15m10086.aspx
Admission to a psychiatric hospital is determined by several factors, including the nature and severity of the illness and the need for safety when the patients are a threat to themselves or others. While all individuals who are hospitalized for a given condition meet some threshold for admission, considerable variability is likely in the state and severity of the patient at presentation. To date, very little investigation into the sociocultural determinants of illness state at the time of hospitalization has been conducted.
Immigration and ethnicity have been shown to be key sociocultural factors in the development and severity of mental illness. The majority of the existing literature, however, has focused on black African and Caribbean populations in the United Kingdom and black African and Latin American populations in the United States, with minimal attention paid to Asian ethnic groups living in western countries. Global migration is an increasingly common phenomenon, with European and North American countries receiving among the highest numbers of international migrants in 2013. In particular, the past few decades have seen a tremendous global diaspora of people of Chinese and South Asian (ie, Indian, Pakistani, Bangladeshi, and Sri Lankan) descent to many western countries; however, little is known about their mental health status. Canada has the highest proportion of foreign-born individuals of any G8 country and has among the largest Chinese and South Asian populations outside of Asia, thus making it an ideal setting to study cross-cultural differences in illness severity.
Despite access to a universal health care system, Chinese immigrants in Canada are far less likely to use mental health services, even among patients with severe and persistent mental illness.
So opens a new paper by Maria Chiu et al., just published in The Journal of Clinical Psychiatry.
Here what they did:
· Data was drawn from the Ontario Mental Health Reporting System (OMHRS), and covered hospital discharges from 1 April 2006 to 31 March 2014.
· The OMHRS data included basic demographic information on patients, as well as DSM-IV diagnoses.
· Inclusion criteria: age over 14, and a hospitalization that was 3 or more days in length, but no longer than 90 days.
· Ethnicity was determined by the ETHNIC database (specificity is 99.7%).
· The authors looked at several measures: involuntary admissions, aggressive behavior (based on the Aggressive Behaviour Scale), the presence of positive symptoms (like hallucinations) and their severity (as determined by the Positive Symptoms Scale).
· Statistical analyses were done.
Here what they found:
· Between 1 April 2006 and 31 March 2014, there were 245,088 unique hospitalizations (excluding ultra-short and long hospitalizations, and inadequate data).
· Patients from these the Chinese and South Asian groups were significantly younger than other populations being hospitalized (42.4 and 41.6, respectively, vs. 45.0 for the reference group).
· The study found that involuntary admissions were significantly more common among Chinese (67.1%) and South Asian (59.7%) patients than among the general population (46%).
· Both groups were also more likely to demonstrate aggressive behaviour (at 20.4% for Chinese and 16.3% for South Asian patients), compared to just 14% among other patients and were more likely to experience multiple psychotic symptoms (55%, 49%, versus 38%).
· Considering odds ratios: “Multivariable adjusted odds ratios stratified by sex showed that the relationship between ethnicity and disease severity were largely the same magnitude between men and women, except among South Asian men (OR=1.21) who showed a trend toward elevated aggressiveness compared to their female counterparts (OR = 0.98).”
· The authors looked at different illnesses — Schizophrenia, Depression, Bipolar — finding a similar pattern.
They note:
In this large, population-based study in Ontario, Canada, we found significant differences in the severity of mental illness among Chinese and South Asian inpatients. In general, illness severity was greatest among the Chinese, followed by South Asians, and the general population, independent of diagnosis. Within each diagnostic category, Chinese patients were more likely to be involuntarily admitted, to exhibit aggressive behaviors, and to present with more positive symptoms than the reference group. The association between ethnicity and illness severity was largely consistent between sexes and across most immigrant categories. Chinese and South Asian ethnicities remained strong risk factors for severe mental illness among those whose index hospitalization was their first encounter with the hospital system.
The authors go on to consider why this was.
The reasons for the greater illness severity at presentation are unclear but are most likely explained by a combination of patient/family factors and health system/provider factors.
Among them: “Higher rates of illness severity can be conceptualized as a consequence of limited access to primary health care or community-based services… Our findings suggest a progression of illness severity associated with a delay in seeking help.” And they argue: “Health system/provider factors including logistic barriers, such as language barriers; culturally insensitive health services; and cultural mismatch between service providers and patients have been proposed as explanatory factors for ethnic differences in the use of mental health care.”
A few thoughts:
First, this is a good paper.
I’ll also note that the authors did an excellent job of not only showing that Chinese and South Asian people were more likely to be admitted involuntarily (odds ratios of 1.79 and 1.31, respectively – wow), but were more ill than the reference group. This wasn’t a single finding, but was remarkably stable across different illnesses and different measures (positive symptoms, agitated behaviour, etc.).
(As an aside, my colleague Dr. Karen Shin, an inpatient psychiatrist at The Scarborough Hospital, wonders about other ethnic groups, like African Canadians, and what patterns could be found – greedily, we can hope for future research.)
Of course, this raises larger questions. Start with the most basic one: Why? As I’ve already noted, the authors didn’t forward one explanation, but several. And that seems about right; there are numerous factors, touching on access, stigma, and larger cultural issues. There is no one cause – but there certainly is one clear pattern.
What then are the implications for service delivery? Study co-author, psychiatrist, and ICES scientist Paul Kurdyak told the Toronto Star:
The longer mental illness goes without treatment, the more difficult it can be to get people back on track. This study highlights that ethnicity and culture are factors that should be considered when developing outreach strategies and treatment approaches, particularly at earlier stages before a patient’s illness worsens and hospitalization becomes necessary.
That makes sense. It speaks to larger issues about funding – we spend just 7 cents on every health dollar in Canada, as opposed to 12 cents, like the UK – but it also speaks to larger issues about organization. To better reach Chinese and South Asian people with mental illness – and, of course, other groups – a traditional bricks-and-mortar outpatient service will fall short.
Our task is great. And will require some creativity.
Reading of the Week. Every week I pick articles and papers from the world of Psychiatry.



Recent Comments