From the Editor
How do we get doctors to practice better medicine?
Here’s a simple idea: what if we send them a sternly written letter? In this week’s Reading, we consider a paper by Columbia University’s Adam Sacarny and his co-authors who did just that. Targeting primary care physicians who were heavily prescribing quetiapine (or Seroquel), they looked at the effects of letters written by government officials, comparing prescribing habits of these physicians with their peers. The result? In the new JAMA Psychiatry paper, they find that prescriptions of quetiapine dropped markedly.
A little nudge, better care?
The core of the idea is that a nudge – that is, the behavioural economic idea of a positive reinforcement and/or an indirect suggestion – can change outcomes. In this Reading, we consider doctors and nudges (and behavioural economics). We also look at a recent study on opioid prescribing, also involving letters.
DG
“Effect of Peer Comparison Letters for High-Volume Primary Care Prescribers of Quetiapine in Older and Disabled Adults: A Randomized Clinical Trial”
Adam Sacarny, Michael L. Barnett, Jackson Le, Frank Tetkoski, David Yokum, Shantanu Agrawal
JAMA Psychiatry, 1 August 2018 Online First
https://jamanetwork.com/journals/jamapsychiatry/article-abstract/2694814
Every year, millions of older adults are prescribed atypical antipsychotic agents for off-label use beyond the indications approved by the US Food and Drug Administration (FDA), which are limited to schizophrenia, bipolar disorder, and some cases of depression. Off-label prescribing to older adults for other indications, such as behavioral symptoms in dementia, anxiety, and insomnia, has continued despite a large body of evidence that the use of atypical antipsychotics is associated with significant harm in these populations. These harms include a host of adverse outcomes, such as increased risk of death, cognitive decline, extrapyramidal symptoms, and sedation.
This evidence has contributed to a broad consensus among psychiatric experts that excessive off-label use of antipsychotic medications in older adults, particularly those with dementia, is a serious problem. Multiple Choosing Wisely recommendations from the American Psychiatric Association target off-label use of antipsychotics. The FDA has warned against the use of antipsychotics for the treatment of elderly individuals with dementia. The American Geriatrics Society recommends that these drugs be used only when other interventions have failed and the patient threatens self-harm or harm to others
Quetiapine fumarate is an atypical antipsychotic that is prescribed at a particularly high frequency for off-label use. In the United States, 2.8 million patients fill a prescription for quetiapine annually, but as much as 75%of quetiapine prescribing lacks a basis in clinical evidence, making it an attractive target for interventions to reduce off-label prescribing.
The widespread off-label use of antipsychotics in spite of clear guidelines has attracted the attention of the Centers for Medicare & Medicaid Services (CMS) and federal oversight agencies. However, there is a gap between the need to curb antipsychotic overprescribing and the evidence base of effective interventions to change prescriber behavior. One existing approach focuses on changing health care professionals’ beliefs about the clinical benefits of prescribing; this intensive education can raise the quality of psychiatric medication prescribing. Another set of techniques based on behavioral economics involves harnessing peer comparison messaging to nudge physicians to change behavior without financial incentives. Yet, there is limited evidence on bringing health care professional education or behavioral nudges to a national scale. To our knowledge, no large-scale randomized behavioral interventions have targeted antipsychotic prescribing. We performed a randomized clinical trial (intent to treat) of peer comparison letters to high quetiapine-prescribing primary care physicians with the goal of reducing excessive prescribing to Medicare program beneficiaries. Because peer comparison letters are inexpensive and easily scaled, they could be a powerful approach to improve the safety of antipsychotic prescribing.
 Adam Sacarny
Adam Sacarny
So begins a new paper by Adam Sacarny et al.
Here’s what they did:
- They selected primary care practitioners, not psychiatrists, who were high prescribers of quetiapine (as a generic or brand, in the regular or extended-release formulations). The physicians were classified as high prescribers if they prescribed the medication at the 75th percentile compared to those in their state, but with a multiplier effect (based on the number of prescriptions filled and total days of quetiapine supplied). They drew from Medicare data (covering Americans 65 years old and older) from 2013 and 2014.
- The physicians were randomized into a control (who received a letter about Medicare enrollment) and an intervention group.
- The physicians in the latter group received a letter that “indicated that the prescriber’s quetiapine prescribing was under review by CMS and was extremely high relative to the within-state peers. The text of the letter discussed that high quetiapine prescribing could be appropriate but was concerning for medically unjustified use. The letter encouraged PCPs to review their prescribing patterns and explained that PCPs could expect to receive future communications from CMS.”
- The placebo and intervention letters were mailed in April 2015, and two follow up letters were sent in August and October 2015.
- The primary outcome was total prescribing days nine months after the intervention.
- Various statistical analyses were done, including multivariable linear regression models.
Here’s what they found:
- Demographically, of the 5055 prescribers, their professional backgrounds were general practitioners (4.6%), family doctors (48.0%) and internists (47.4%); the vast majority were male (82.2%).
- “The average prescriber in the study was responsible for supplying 2916 days (97 months) of quetiapine during the 9 months before the intervention (or about 3 months of quetiapine per week). On average, 820 (28.1%) of these days were to patients for likely low-value indications, and 778 (26.7%) were to patients for likely guideline-concordant indications.”
- “During the 9-month postintervention period, the average treatment arm prescriber supplied 2456 days (82 months) of quetiapine vs 2864 days (96 months) in the control arm, an adjusted difference of −319 days… per prescriber or an 11.1%… decrease vs control…” At two years, there was a 15.6% decrease.
- “At the prescriber level, the intervention reduced quetiapine prescribing to both low-value and guideline-concordant patients.” (!!)
- At the patient level: “The intervention was associated with a reduction of 6.7 days of quetiapine… received per patient over 9 months…” That works out to a 3.9% relative decrease.
- This is a good study.
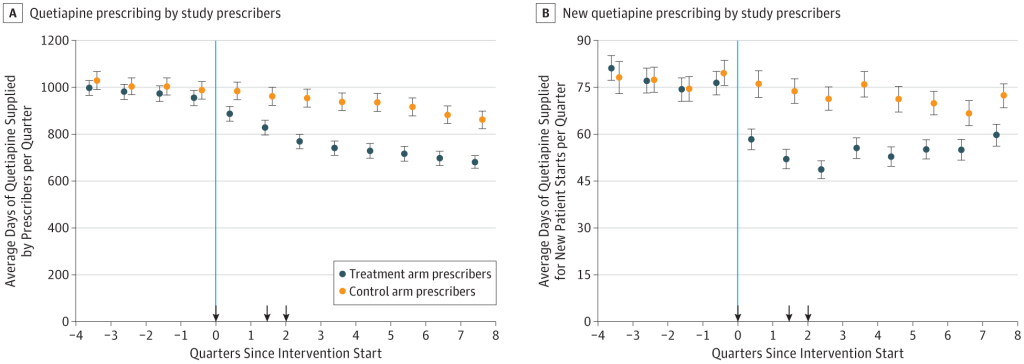
- The letter had an impact. Inappropriate use of quetiapine (prescriptions to what the authors call “low value patients”) went down. Good. But appropriate use of quetiapine (prescriptions to what the authors call “guidance-concordant patients”) also went down. Not so good. See figure below.
- Was this a nudge (to use the behavioural economics term) – or a push? The letter was strongly worded and from a government agency, with the mention of a possible further review.
- There are limitations to this study, including that it drew from Medicare data, but not non-Medicare data. Was the prescribing effect seen for the non-elderly? We don’t know.
- While these results are robust, we can wonder if there would be “warning fatigue” if applied to other medications (think benzodiazepines, other antipsychotics, opioids).
- The paper runs with a thoughtful editorial written by Joshua M. Liao and Amol S. Navathe. “Nudging Physicians to Reduce Quetiapine Prescribing Using Medicare Letters: Following the Letters of the Law?” opens:
Physician decision making is an integral part of nearly every aspect of health care delivery. However, because physicians must synthesize large and growing amounts of clinical data and medical evidence, they frequently rely on heuristics (mental shortcuts) that may lead to predictably irrational decisions. Consequently, improving the value of health care may hinge in part on the ability to improve clinical decision making, particularly where medical evidence clearly identifies appropriate choices. This is the premise behind physician-focused nudges, or interventions that leverage insights from behavioral economics to deliberately adjust how information is presented to physicians to improve their choices.
They note the success of nudging with physician prescribing in other areas:
- “Nudges can reduce opioid prescribing among emergency physicians,reduce inappropriate antibiotic prescribing among primary care physicians,and improve generic medication prescription rates.”
- “Many of these nudges use peer comparisons, a promising approach for influence prescribing behavior by providing physicians with comparative feedback on their own performance compared with that of their peers.”
Intervention letters appeared to be relatively blunt instruments, reducing prescriptions among both guideline-concordant and low-value patients. In turn, access to quetiapine, particularly among guideline-concordant patients for whom the medication may have been appropriate, could have been inappropriately decreased. While some measures suggested a lack of major adverse effects (eg, no increase in emergency department visits), other patient outcomes (eg, quality of life) that were not measured in the trial may have worsened because of reductions in rates of prescription—effects that may not be uncovered because of data access limitations and the inability to conduct additional post hoc analyses.
They go on to argue:
[A]dditional work is needed to understand any negative implications of intervention letters that reduced quetiapine prescriptions among guideline-concordant as well as low-value patients. Though designed to be subtle, nudges can lead to outsized unintended effects, an issue that may be most relevant for interventions aimed at reducing medical overuse or misuse.
- A new paper by Jason N. Doctor et al. considers opioid prescribing in “Opioid prescribing decreases after learning of a patient’s fatal overdose.” In this Science study, physicians received a letter after the death of patient. They find: “Milligram morphine equivalents in prescriptions filled by patients of letter recipients versus controls decreased by 9.7% (95% confidence interval: 6.2 to 13.2%; P < 0.001) over 3 months after intervention.” That paper can be found here: http://science.sciencemag.org/content/361/6402/588.long.
- Past Readings have considered behavioural economics. See the digital archive: http://davidgratzer.com/tag/behavioural-economics/.
Reading of the Week. Every week I pick articles and papers from the world of Psychiatry.



Recent Comments