From the Editor
Lithium is effective as a medication. How often is it prescribed?
This week, there are three selections, and we open with a small paper with a big finding.
In the first selection, Dr. Scott B. Patten and Jeanne V. A. Williams (both of the University of Calgary) draw on national survey data to consider lithium prescribing in Canada. “The frequency of lithium use is surprisingly low,” they find.
 Lithium: on the Periodic Table, but not in the drug cabinet
Lithium: on the Periodic Table, but not in the drug cabinet
In the second selection, we look at a Nature Medicine article that contemplates social media and medical research. Writer Nicole Wetsman quotes Dr. Esther Choo, an emergency physician who is prominent on Twitter: “It’s incredible medical education.”
Finally, for the third selection, we tip our hats to the holiday season, and consider a not-so-new BMJ paper on holiday chocolates. Published as part of a past Christmas issue – the popular, annual tradition that takes a light-hearted approach to inquiry – Bedford Hospital’s Parag R. Gajendragadkar and his co-authors ask a not-so-weighty question: how long do holiday chocolates last on hospital wards?
Note that there will be no Reading next week. Happy Holidays.
DG
Selection 1: “Lithium, an Infrequently Used Medication”
Scott B. Patten and Jeanne V. A. Williams
The Canadian Journal of Psychiatry, 28 November 2019 Online First
![]()
Lithium is recommended as a first-line treatment for bipolar disorder by contemporary clinical practice guidelines. With a prevalence of bipolar disorder believed to be in the range of 1% to 2% in Canada, expectation holds that lithium should be frequently used. However, its use is complicated by the need for safety monitoring and the possibility of adverse events.
The prevalence of lithium use in the Canadian population is unknown. Prescription data are, in principle, available from provincial databases in several provinces, but these do not provide national estimates. In the current study, we sought to estimate the frequency of lithium use in the household population using national survey data.
So begins a short paper by Dr. Patten and Williams.
In this analysis, we used data from two national Mental Health Surveys: the 2002 Canadian Community Health Survey (CCHS) and the 2012 CCHS-MH. We also used estimates from the Canadian Health Measures Survey, pooling two sets of estimates, 2009 to 2011 and 2013 to 2017. The surveys collected medication data by including questions about medication use, including asking respondents to collect and look at the bottles, tubes, or boxes containing their medications.
They use a couple of different statistical analyses to estimate lithium use.
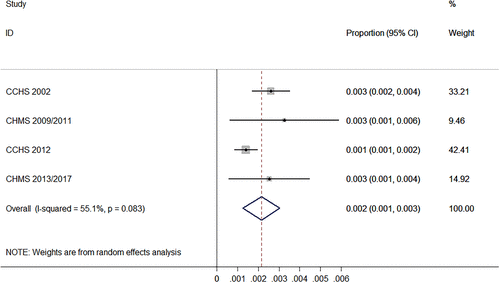
Given the historically central role of lithium in the treatment of bipolar disorders, the frequency of lithium use is surprisingly low, although the estimates presented here resemble those previously reported for Denmark (0.17%), Norway (0.21%), and Sweden (0.25%).
The authors consider several explanations.
It is conceivable that the observed frequencies represent an optimal frequency of lithium utilization based on its tolerability and effectiveness. However, there is also the possibility that the inconvenience associated with laboratory monitoring, exaggerated safety concerns, or a lack of familiarity with this medication among clinicians is resulting in underuse of the medication. Access to psychiatric care may be another factor, since nonpsychiatrist prescribers may be especially hesitant to use lithium.
This paper is short but important. Lithium has advantages over other first line medications used to treat bipolar, but the prescribing habits don’t reflect that; relatively few patients use lithium. In other words, lithium, like other highly evidenced treatments – think clozapine and ECT – is underutilized here (and in other countries). The authors offer a few credible explanations.
Quick questions: Is this a failure of training? Do we need to educate residents of psychiatry and family medicine better?
https://journals.sagepub.com/doi/full/10.1177/0706743719890714
Selection 2: “How Twitter is changing medical research”
Nicole Wetsman
Nature Medicine, 9 December 2019

Esther Choo only had a few thousand followers on Twitter before August 2017. Choo, an emergency physician at the Oregon Health & Science University, interacted mostly with other doctors. But when she tweeted one day about the racism she had endured while practicing medicine, her posts went viral – and her follower count shot up to 20,000 almost overnight. Now, she has nearly 80,000 followers.
‘The professional benefits have been so concrete,’ Choo says. Twitter, for her, has helped her meet new professional colleagues and friends and has offered opportunities for advocacy around racial and gender equity in medicine. ‘It’s hard to imagine what my career would be like without it.’
As a high-profile physician on the platform, Choo (@choo_ek) is an outlier in the medical community terms of her number of followers – but she’s part of a large and growing community of doctors and scientists who use Twitter as part of their professional lives.
So begins an article by Wetsman.
After noting the opportunity that social media offers the platform for activism for physicians like Dr. Choo, she explores several aspects of social media and medical research:
- Debate in real time. “Before Twitter, researchers had limited ways to respond to and critique new research in their field. They could write a letter to the editor or an opinion piece in a journal, but that response would be published only if editors of that journal agreed to it. Even if it was published, it would often not appear for weeks.”
- Twitter for education. “Online discussion of papers is sometimes facilitated by Twitter journal clubs. Journal clubs, where researchers get together and critically examine new papers or pieces of literature, are important forums for the exchange of ideas and continuing education. But they traditionally happen in person, and participants are usually limited by location. On Twitter, however, journal clubs can expand beyond those boundaries.”
- Opening up the discussion. “On Twitter, people who do not have tenure, or have more limited publications to their name, or are early in their career have opportunities to demonstrate their expertise. But displays of knowledge on social media, rather than in traditional forums like journals, are sometimes criticized as less relevant or rigorous.”
Wetsman does note that social media is changing the world of medical research – and not necessarily always for the better. Online discussions can be caustic, especially for new papers. Dr. Jordan Gauthier of the Fred Hutchinson Cancer Research Center notes: “You can see sharks gathering around a paper to tear it apart.” Wetsman also cites a study finding that the majority of scientists aren’t on Twitter.
The article is balanced and thoughtful. While social media is often used for less important things, some see a role in the dissemination and discussion of medical literature. Not surprisingly, major journals have noticed, and often tweet about new studies. I was speaking recently with the editor of The British Journal of Psychiatry who argues that social media is an important way of reaching people who don’t ordinarily read papers, such as members of the public and policy makers.
It seems that there is more to social media than presidential rants and cat videos.
https://www.nature.com/articles/s41591-019-0697-7
Selection 3: “The survival time of chocolates on hospital wards: covert observational study”
Parag R. Gajendragadkar, Daniel J. Moualed, Phillip L. R. Nicolson, Felicia D Adjei, Holly E. Cakebread, Rudolf M. Duehmke, Claire A. Martin
BMJ, 14 December 2013

A higher chocolate consumption has been linked with reduced risks for the development of cardiometabolic disorders. The authors’ experience is that chocolate consumption in a hospital environment is a relatively common occurrence, and that gifts from patients and their families represent a large proportion of healthcare workers’ chocolate consumption. Subjectively, we noted that chocolate boxes emptied quickly and that determining which healthcare professionals ate the most chocolates was a common source of workplace conflict. Literature on chocolate consumption by healthcare workers in a hospital setting is lacking.
We carried out an exploratory study to provide quantitative data on patterns of chocolate consumption in a hospital environment. Specifically we estimated the survival time of a chocolate in a ward setting, modelled mathematically any pattern of chocolate consumption observed, estimated if survival time was affected by chocolate brand, and investigated differences in healthcare professionals’ chocolate consumption stratified by job type.
So begins a paper by Dr. Gajendragadkar et al.
Yes, the paper is on chocolate – and, yes, it’s highly entertaining.
Here’s what they did:
- “The study was prospective and conducted across three UK sites and four different wards.”
- “At approximately 10 am an observer (a doctor who was familiar with the ward in which testing was being carried out) covertly placed the boxes side by side in a prominent location in the main nursing or reception area, where such gifts are normally placed. The observers covertly recorded what time each box was opened, and at what time individual chocolates were taken from each box.”
- “We chose to study a 350 g box of Quality Street chocolates (Nestlé, Switzerland) and a 350 g box of Roses chocolates (Cadbury, United Kingdom), on the basis that they are commonly given as gifts and are two of the leading brands of chocolates available in the United Kingdom and elsewhere.”
- “Pilot data investigating a range of brands showed that these two contained similar numbers of chocolates (between 30 and 35 on average).”
- “The primary outcome was the median survival time of a chocolate.”
- Statistical analyses were done.
Here’s what they found:
- “Overall, 191 chocolates out of a possible 258 (74%) were observed to have been eaten. The remainder were left over and lost to follow-up. The mean observation period was 254 minutes (95% confidence interval 179 to 329). No adverse events occurred.”
- “The median survival time of a chocolate was 51 minutes (95% confidence interval 39 to 63).”
- “Regression curve fitting suggested that the rate of emptying of a box of chocolates was best explained by an exponential decay curve with equation Cp=e−λt; where Cpis the proportion of chocolates remaining, t is the time in minutes, and λ is the decay constant…”
- “Quality Street chocolates survived longer than Roses chocolates…”
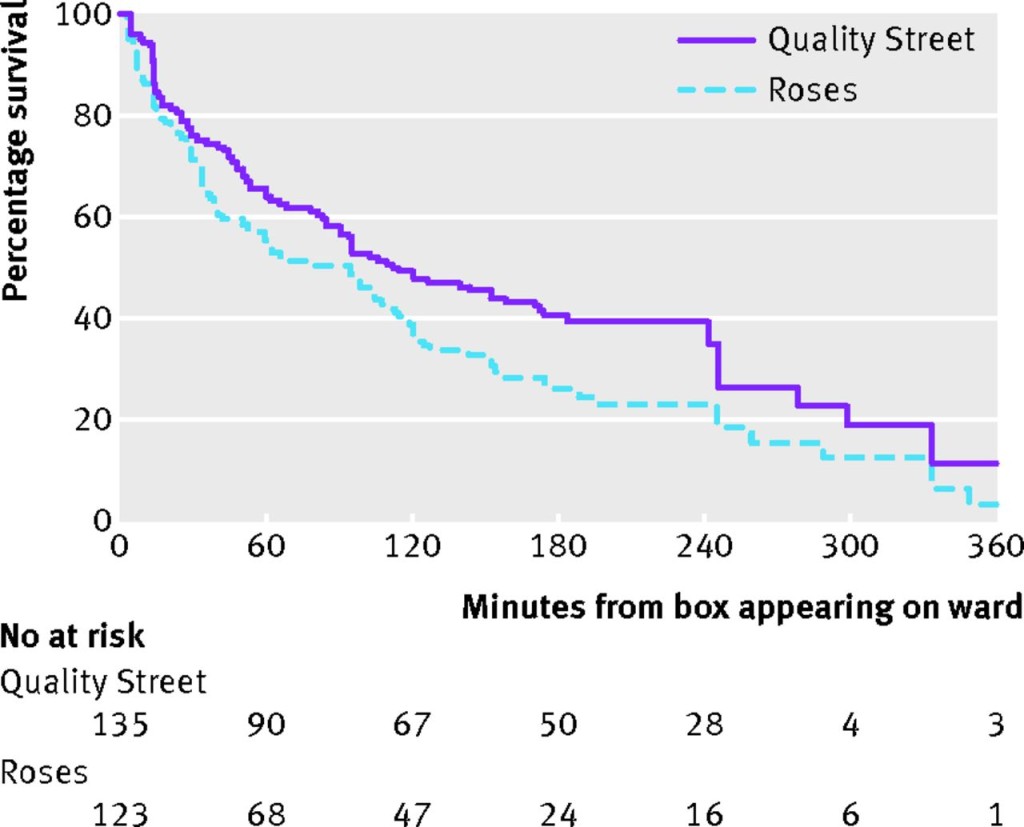
Chocolates left on wards for staff are consumed rapidly. An exponential decay model best explained how a box of chocolates was consumed in a ward environment.
For the record, this year’s BMJ Christmas issue will be released tomorrow – just one sleep away.
https://www.bmj.com/content/347/bmj.f7198
Reading of the Week. Every week I pick articles and papers from the world of Psychiatry.
Recent Comments